Essay about Family: What It Is and How to Nail It

Humans naturally seek belonging within families, finding comfort in knowing someone always cares. Yet, families can also stir up insecurities and mental health struggles.
Family dynamics continue to intrigue researchers across different fields. Every year, new studies explore how these relationships shape our minds and emotions.
In this article, our dissertation service will guide you through writing a family essay. You can also dive into our list of topics for inspiration and explore some standout examples to spark your creativity.

What is Family Essay
A family essay takes a close look at the bonds and experiences within families. It's a common academic assignment, especially in subjects like sociology, psychology, and literature.
.webp)
So, what's involved exactly? Simply put, it's an exploration of what family signifies to you. You might reflect on cherished family memories or contemplate the portrayal of families in various media.
What sets a family essay apart is its personal touch. It allows you to express your own thoughts and experiences. Moreover, it's versatile – you can analyze family dynamics, reminisce about family customs, or explore other facets of familial life.
If you're feeling uncertain about how to write an essay about family, don't worry; you can explore different perspectives and select topics that resonate with various aspects of family life.
Tips For Writing An Essay On Family Topics
A family essay typically follows a free-form style, unless specified otherwise, and adheres to the classic 5-paragraph structure. As you jot down your thoughts, aim to infuse your essay with inspiration and the essence of creative writing, unless your family essay topics lean towards complexity or science.
.webp)
Here are some easy-to-follow tips from our essay service experts:
- Focus on a Specific Aspect: Instead of a broad overview, delve into a specific angle that piques your interest, such as exploring how birth order influences sibling dynamics or examining the evolving role of grandparents in modern families.
- Share Personal Anecdotes: Start your family essay introduction with a personal touch by sharing stories from your own experiences. Whether it's about a favorite tradition, a special trip, or a tough time, these stories make your writing more interesting.
- Use Real-life Examples: Illustrate your points with concrete examples or anecdotes. Draw from sources like movies, books, historical events, or personal interviews to bring your ideas to life.
- Explore Cultural Diversity: Consider the diverse array of family structures across different cultures. Compare traditional values, extended family systems, or the unique hurdles faced by multicultural families.
- Take a Stance: Engage with contentious topics such as homeschooling, reproductive technologies, or governmental policies impacting families. Ensure your arguments are supported by solid evidence.
- Delve into Psychology: Explore the psychological underpinnings of family dynamics, touching on concepts like attachment theory, childhood trauma, or patterns of dysfunction within families.
- Emphasize Positivity: Share uplifting stories of families overcoming adversity or discuss strategies for nurturing strong, supportive family bonds.
- Offer Practical Solutions: Wrap up your essay by proposing actionable solutions to common family challenges, such as fostering better communication, achieving work-life balance, or advocating for family-friendly policies.
Family Essay Topics
When it comes to writing, essay topics about family are often considered easier because we're intimately familiar with our own families. The more you understand about your family dynamics, traditions, and experiences, the clearer your ideas become.
If you're feeling uninspired or unsure of where to start, don't worry! Below, we have compiled a list of good family essay topics to help get your creative juices flowing. Whether you're assigned this type of essay or simply want to explore the topic, these suggestions from our history essay writer are tailored to spark your imagination and prompt meaningful reflection on different aspects of family life.
So, take a moment to peruse the list. Choose the essay topics about family that resonate most with you. Then, dive in and start exploring your family's stories, traditions, and connections through your writing.
- Supporting Family Through Tough Times
- Staying Connected with Relatives
- Empathy and Compassion in Family Life
- Strengthening Bonds Through Family Gatherings
- Quality Time with Family: How Vital Is It?
- Navigating Family Relationships Across Generations
- Learning Kindness and Generosity in a Large Family
- Communication in Healthy Family Dynamics
- Forgiveness in Family Conflict Resolution
- Building Trust Among Extended Family
- Defining Family in Today's World
- Understanding Nuclear Family: Various Views and Cultural Differences
- Understanding Family Dynamics: Relationships Within the Family Unit
- What Defines a Family Member?
- Modernizing the Nuclear Family Concept
- Exploring Shared Beliefs Among Family Members
- Evolution of the Concept of Family Love Over Time
- Examining Family Expectations
- Modern Standards and the Idea of an Ideal Family
- Life Experiences and Perceptions of Family Life
- Genetics and Extended Family Connections
- Utilizing Family Trees for Ancestral Links
- The Role of Younger Siblings in Family Dynamics
- Tracing Family History Through Oral Tradition and Genealogy
- Tracing Family Values Through Your Family Tree
- Exploring Your Elder Sister's Legacy in the Family Tree
- Connecting Daily Habits to Family History
- Documenting and Preserving Your Family's Legacy
- Navigating Online Records and DNA Testing for Family History
- Tradition as a Tool for Family Resilience
- Involving Family in Daily Life to Maintain Traditions
- Creating New Traditions for a Small Family
- The Role of Traditions in Family Happiness
- Family Recipes and Bonding at House Parties
- Quality Time: The Secret Tradition for Family Happiness
- The Joy of Cousins Visiting for Christmas
- Including Family in Birthday Celebrations
- Balancing Traditions and Unconditional Love
- Building Family Bonds Through Traditions
Looking for Speedy Assistance With Your College Essays?
Reach out to our skilled writers, and they'll provide you with a top-notch paper that's sure to earn an A+ grade in record time!
Family Essay Example
For a better grasp of the essay on family, our team of skilled writers has crafted a great example. It looks into the subject matter, allowing you to explore and understand the intricacies involved in creating compelling family essays. So, check out our meticulously crafted sample to discover how to craft essays that are not only well-written but also thought-provoking and impactful.
Final Outlook
In wrapping up, let's remember: a family essay gives students a chance to showcase their academic skills and creativity by sharing personal stories. However, it's important to stick to academic standards when writing about these topics. We hope our list of topics sparked your creativity and got you on your way to a reflective journey. And if you hit a rough patch, you can just ask us to ' do my essay for me ' for top-notch results!
Having Trouble with Your Essay on the Family?
Our expert writers are committed to providing you with the best service possible in no time!
FAQs on Writing an Essay about Family
Family essays seem like something school children could be assigned at elementary schools, but family is no less important than climate change for our society today, and therefore it is one of the most central research themes.
Below you will find a list of frequently asked questions on family-related topics. Before you conduct research, scroll through them and find out how to write an essay about your family.
How to Write an Essay About Your Family History?
How to write an essay about a family member, how to write an essay about family and roots, how to write an essay about the importance of family.

Daniel Parker
is a seasoned educational writer focusing on scholarship guidance, research papers, and various forms of academic essays including reflective and narrative essays. His expertise also extends to detailed case studies. A scholar with a background in English Literature and Education, Daniel’s work on EssayPro blog aims to support students in achieving academic excellence and securing scholarships. His hobbies include reading classic literature and participating in academic forums.

is an expert in nursing and healthcare, with a strong background in history, law, and literature. Holding advanced degrees in nursing and public health, his analytical approach and comprehensive knowledge help students navigate complex topics. On EssayPro blog, Adam provides insightful articles on everything from historical analysis to the intricacies of healthcare policies. In his downtime, he enjoys historical documentaries and volunteering at local clinics.
.webp)
- Essay Samples
- College Essay
- Writing Tools
- Writing guide

↑ Return to College Essay
Essay about family tree – Research essay
Introduction
In my research paper, I have studied my family tree and have turned up information about people in my family. This information includes things that appear to define them or their character today and/or in the past. Thelma Griffin: mother of Peter Griffin
The line starts with Thelma Griffin. This is as far back as I could go at this present time. Thelma was the mother of me Peter, and she spent her early years as a waitress and then became a professional gambler. She met my father Mickey during a trip to Ireland where I was conceived. She returned to America shortly after, which is where I was born. Mickey McFinnigan: father of Peter Griffin
A man of Irish blood, he is still a much-respected town drunk in a small Irish village. He has never visited the USA and was unaware of my birth for many years. Peter Griffin: me
I am currently a mature student trying to earn my degree in sociology. I have three children, though it is possible that I have more that I am unaware of. I have a wife called Lois Pewterschmidt. Barbra Hebrewberg: mother of Lois
Barbra is married to Cater Pewterschmidt, and is a wealthy New England mother of Jewish heritage. She is the mother to Lois my wife, to Carol Pewterschmidt and the disowned Patrick Pewterschmidt.
Carter Pewterschmidt: father of Lois
Carter is a New England millionaire and managing director of Pewterschmidt industries. He is a strict Christian and was unaware of his wife’s Hebrew background until years after marrying her.
Stewart Griffin: my son
He is almost two years old and is very advanced for his age. He has already had a short career on stage with a child slightly older than him, and in his short life has visited eleven countries. Meg Griffin: my daughter
She is an 18-year-old girl that is currently in college. She is generally unpopular although is pure of heart and unfairly treated by most people because she is a plump and unattractive girl that wants to fit in.
Chris Griffin: my son Chris has a very low IQ and has been held back in high school to help him eventually graduate. He is sixteen and has had reasonable success in finding and keeping jobs, though is accident prone and easily fooled. Carol Pewterschmidt: sister of Lois
Carol’s defining feature is that she has had over 15 marriages break down, though she is now married to the Mayor of Quahog, a small New England town.
Patrick Pewterschmidt: brother to Lois
He was abandoned at a young age and sent to a psychiatric facility where he still remains. He is believed to have committed heinous crimes due to his inability to get over a childhood trauma that involved a very fat man.
Though my family tree is not a big one, though there are far more entries to it. The family tree I have created goes as far back as I can go given the resources at my disposal.

Follow Us on Social Media
Get more free essays

Send via email
Most useful resources for students:.
- Free Essays Download
- Writing Tools List
- Proofreading Services
- Universities Rating
Contributors Bio

Find more useful services for students
Free plagiarism check, professional editing, online tutoring, free grammar check.
Alex de Fircks

How families are like trees – a metaphor still used today
- May 30, 2021
- Family , History , Moments in Time , von Fircks
I love family trees. One can gather so much information from them if they have been done correctly. And if there are blanks, that just means there is so much more to research and discover – so many opportunities to disappear down multitudes of rabbit holes. Bliss!
“Like a tree, a family is born, flourishes, branches out, and withers. This metaphor haunted pictorial representations of kinship for centuries until it finally assumed the fixed image of ‘the family tree’,” so writes Christiane Klapisch- Zuber in an essay about the origins of the family tree as we know it today. [1] I guess some families, just as some trees, take longer than others to either flourish or wither. According to Klapisch-Zuber, family trees did not begin to be produced in the form we would recognise today until the 15 th century, becoming the fashion, especially among European influential families, in the second half of the 16 th century. This was despite families and trees having been compared to each other in a genealogical sense for some time before that.
In fact, according to Klapisch-Zuber, the last years of the 12 th century saw genealogy become the most accurate way of maintaining not only the memory of one’s ancestors, but also the reputation of one’s family line. The recording of one’s genealogy also provided a means of distributing property – naturally only through the male line.
The picture above shows an early version of the Fircks family tree. It has been taken from the genealogical record of the von Fircks family compiled by my cousin Wolf Lackschewitz. Thanks to the research and work undertaken by Wolf, who has since passed away, I have a wonderful insight into my paternal family history. The inscription underneath translates to: The family tree submitted by Christopher I (died 1649) at the time of registration for the 1620 matriculation (register). The original can be found in the Herder Institute in Marburg, Germany. It is the earliest depiction of the Fircks family tree that I know of. I just wish I could read the names on it!
Christopher I is one of my direct ancestors. It was his father Jürgen (or Georg) who originally bought the village of Nurme and built the family estate Nurmhusen, which I have previously written about here. Christopher was the eldest child of Jürgen and his second wife Elizabeth who died in 1570. I cannot find a birth date for Christopher, but apparently the first mention of him was in 1582. He inherited Nurmhusen after his father died in 1600.
I doubt the wording under the family tree means matriculation in the sense of schooling as we would think of it. In October of 1620, the von Fircks family, with Christopher as its head, was listed in the Kurland Electoral Register of the Nobility – and I believe this is the reason he had to produce the family tree.
[1] Klapisch-Zuber, Christiane. “The Genesis of the Family Tree.” I Tatti Studies in the Italian Renaissance 4 (1991): 105-29. Accessed May 30, 2021. doi:10.2307/4603672.
Share this article:
- Tags: Family , Family history , Family tree , Kurland , Metaphor , Nurmhusen , von Fircks

You Might Also Like:

- Searching for the graves of my ancestors can literally lead to dead ends!
My latest search is for the graves of my maternal great grandmother and three of her daughters, my great aunts. My maternal great grandmother, Catherine

- What’s in a Name – quite a bit if you are a family historian!
“Wot’s in a name? she sez. An’ then she sighs, An’ clasps ‘er little ‘ands, an’ rolls ‘er eyes. A rose, she sez, be any

- How Betty Crocker inspired my mother and how my mother inspired my love of cooking
One of the books I inherited from my mother is falling apart. The covering of the spine has been lost, the edges of the pages
Leave a Reply Cancel reply
Recent posts.
- Take note of what the King said – he had useful advice about beginning
- 5 Ways I Discovered More About My Family History
Subscribe to Blog via Email
Email Address
Recent Comments
- Alex on Nurmhusen, my father’s family estate
- Juris on Nurmhusen, my father’s family estate
- Alex on Searching for the graves of my ancestors can literally lead to dead ends!
- Jim Renes on Searching for the graves of my ancestors can literally lead to dead ends!
Project Types We Cover
- Admissions Essay
- PowerPoint Presentation
- Research Paper
- Book Reviews
- Personal Statement
- Ph.D Dissertation
- Proofreading
Academic Fields & Subjects
- Programming
- Computer Science
- Other projects we help with
- Our Experts
- Plagiarism Checker
- Writing Tips
- Essay Writing on My Family
How Should I Go About Writing My Family Essay?: Examples and Tips
By: Angelina Grin

It can be intimidating to write a paper about family. Essay writing is difficult enough on its own, but you may think, “When writing about my family, essay research and writing will feel so personal.” Our family memories are some of the most personal we have; they shape how we see and interpret the world. How can something so intimate be distilled into a meaningful piece of writing?
In this article, we’ll cover tips for writing an essay about family. We’ll also offer an example essay about family.
Writing a family essay, whether for a class, a personal essay contest , or a memoir, may be a challenging task. So, let's figure out how to write this specific type of essay, and if you need a simple how-to write any essay guide, check out our article.
How to Write an Essay About My Family in English
What topics should i write about for my family essay, 1. writing a family tree, 2. describing my family in my essay, 3. writing about a personal memory, example: my family and i essay in 500 words, describe your family: essay example in ten lines, dos and don’ts when writing a family stories essay, what is a good hook for an essay on my family, what should i include in an essay about me and my family, how should i start an essay all about my family, how long should my essay about my family be.
Why would someone want to write an essay about family? It could be for a variety of reasons. Perhaps it's for a school project. Perhaps it's a personal essay competition entry. Maybe it's for a memoir. Whatever your motivation for creating a piece about family, essay writing can be difficult, and you may be unsure where to begin.
If you’ve ever wondered, “How can I write an essay about myself and my family?” this section is for you. Read on for some essential steps:
- Research and brainstorm. The first step for any piece of writing should be research. Take some time to interview your family members, or even do some introspection before you start the writing process. If you are writing about an event, you personally experienced, you could read old journal entries or look through old photos to jog your memory.
- Outline your paper. Once you’ve researched and decided on a topic for your essay, it’s time to start working on an outline. Decide how you will present your topic to the reader in the introduction and give some thought to the material that will go into the main paragraph. You should write about memories or family members that relate to your theme.
- Begin writing. With your outline prepared, you can now start writing. Your first draft isn’t going to be perfect, so just try to get everything down on the page. Multiple drafts of your paper are an excellent approach to polishing your work.
- Proofread and edit your work. Once you’ve completed the final draft of your essay, carefully read through it for mistakes. Make whatever edits are necessary, and take the time to see if there are any finishing details you could add to your paper to really make it shine.
Papers about your family can be a useful space to explore your relationship with them and to reflect upon what they mean to you and what they’ve taught you.
So, what comes to mind while considering an essay topic about family? Whatever you choose should be something that you feel strongly about. Personal essays are more than just dry, factual accounts of events; they should also have a deeper meaning or message.
Here are a few examples of the types of topics you can focus on when composing an essay about a family or family event:
A conflict. Conflict can provide us with a greater insight into our relationships. In fiction, all interesting stories are based on some type of conflict. So too personal essays that deal with conflict can be some of the most interesting works of reflective writing.
Example: My father and I get along great for the most part, but we sometimes struggle to reconcile our political differences. He has always been a staunch Republican whereas I am a Democrat; we just can’t seem to agree to disagree. After a particularly bad fight one year at Christmas, we’ve decided it’s better if we stay away from the topic of politics.
An influential family member. Perhaps you have an uncle who helped shape your career or introduced you to a hobby that you’ve grown to love over time. Perhaps a favorite grandparent gave you a life-changing piece of advice that you still carry with you years later. Perhaps one day you got into a fight with a sibling that forever changed the trajectory of your relationship. Essays that talk about your family’s influence on your personality, life, and decisions can be very compelling.
Example: My uncle is a dentist. No one likes going to the dentist, but Uncle Mark can instantly put people at ease, even kids. He heals with a smile and helps the people who come to his office leave feeling confident. It was his attitude and effect on people that inspired me to follow in his footsteps and become a dentist.
Values your family has instilled within you. You might also choose to write about particular values your family placed in you. Our families help shape the fundamental building blocks of who we are and how we think. Exploring this through writing can produce an interesting paper.
Example: My mom has always believed in broken windows theory. As a result, we were taught from a young age how to keep our home clean and safe and were shown how important it was to take care of our surroundings. I may have rolled my eyes at her sometimes when I was young, but now that I’m older and more sensible I appreciate those lessons.
This is just a small handful of ideas to help get you thinking about your essay, but there are many more topics you could choose to write about.
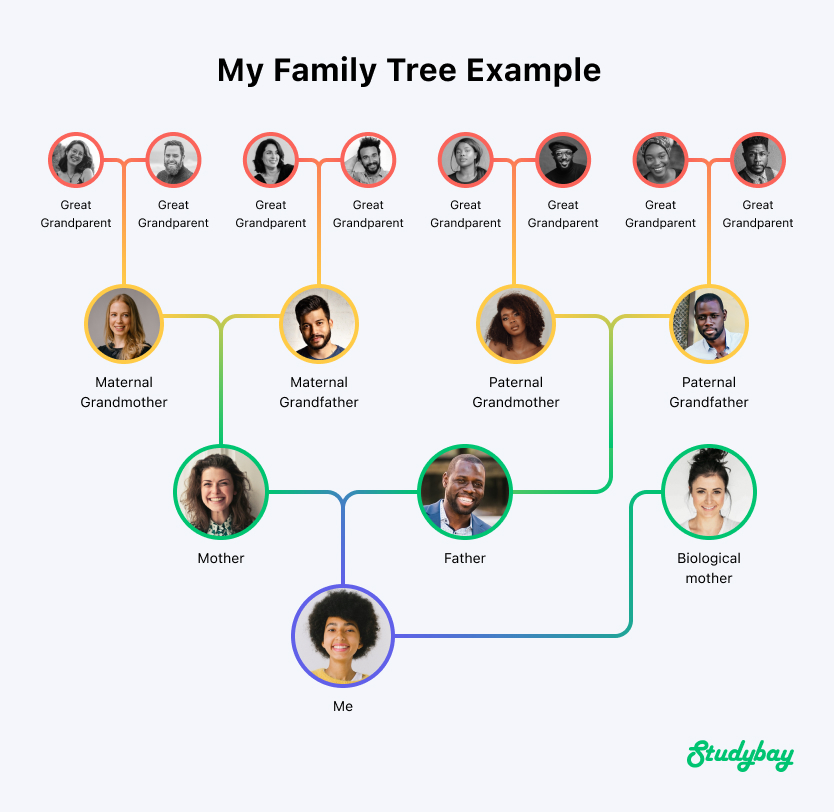
If you’re writing a piece that deals with your lineage, composing a family tree can be a useful exercise before you start writing. You might choose to conduct research on your own or reach out for help. It’s entirely up to you. Just make sure your work is accurate and thorough.
You might choose to build this chart using an online tool. Once it’s completed, you can print it off so that you have a physical copy. You might even write it out by hand. It can be useful to map it out on a large piece of card and pin it to your wall, ideally near where you’ll be doing your writing.
Once your chart is drawn up, you can use it to inspire your essay. Try to come up with stories involving different people that somehow connect to the main theme of your piece. If it’s helpful, you could brainstorm ideas using spider diagrams, making lists, or whatever other option works for you.
When you’re raised in a group of people, it may feel like you know everything about them there is to know. But you’d be surprised to find out all you don’t know! Older ones can be a font of experiences and memories. If you’re comfortable approaching them, and if they’re happy to have their experiences recorded in your work, you might interview them to help flesh out your essay. You could even quote them in your paper.
Once you’ve done all the research you need—assembled your family tree, carried out interviews, consulted public records—it’s time to start writing. But you might wonder how to describe your family in an essay.
Consider the following tips for selecting details about your relatives to add to your family article:
- Remember, your essay should serve a particular theme or idea. Keep this in mind throughout the whole writing process, but especially during the planning phase when you're deciding which details to add.
- Don’t clutter your essay with lots of irrelevant details. For instance, if you’re writing about how your mother motivated you to pursue a career in medicine, it makes more sense to talk about how she influenced you—for example, by being passionate, compassionate, and helpful—rather than having a random piece about an unrelated hobby she has.
Furthermore, how do you know what level of detail is appropriate for your work? Here are some suggestions:
- Especially if you intend for your essay to be published, whether online or in a physical format, you should consider your family’s feelings. Hopefully, you’ve already asked for consent from them to talk about the personal details of your life. But you should also be conscientious during the writing process. If you’re discussing a sensitive part of your family history, make sure to use tact.
- You should also consider how much detail you include from a writing perspective. Think of fleshing out your family members as you would think of fleshing out characters in a novel. You should describe their sensibilities and the personality traits that define them. You could also include physical descriptions if you thought that might add something to your essay.

When you’re writing an essay about the family, or indeed any other kind of personal essay, drawing on personal memories is an invaluable way of bringing your writing to life and making your paper resonate with your reader. Even if you’re writing about a rather unique sequence of events that your reader hasn’t been through, a well-written personal memory can help place them in your shoes.
So, how can you effectively write about a personal memory? Here are some tips to get you started:
Consider how the memory services the overall themes of the essay. Our lives are composed of countless little moments, interspersed with grand, life-changing events. Whether you’re writing about something small and apparently inconsequential or something big that forever altered the trajectory of your life, make sure it’s relevant to your theme.
Example: Pursuing a career in music is not easy, but it’s something I’ve always felt meant to do. Perhaps that’s because I was always surrounded by musicians growing up. My parents both played piano, and I remember coming downstairs on a Saturday morning to the smell of brewing coffee and the sound of my parents dueting on the piano.
Make use of memory triggers. When you’re getting ready to write, make use of memory triggers to put you back in the moment. What do we mean by memory triggers? This can be anything from the music you associate with the memory, photographs taken at the time, or even smells or foods linked with the event.
Example: When I was a young girl, I went on a trip to the beach with my family. I was very young at the time, so I don’t have a very clear memory of it, but I will always associate that seaside visit with the taste of pink lemonade. We passed around bottles of it as we made castles in the sand. To this day, that drink always reminds me of summer.
Use sensory descriptions. To carry on from our last tip, use sensory descriptors when you’re writing personal memories. Always keep the five senses in mind: sight, hearing, touch, smell, and taste. A useful exercise before working on your essay can be to write a couple of paragraphs just focusing on the sensations you remember. Don’t worry about telling a story or recording dialogue. Just place all your focus on remembering how you felt at the time and describing these sensations as vividly as possible.
Example: My uncle and aunt often took my cousins and me hiking when I was growing up. Once, we climbed Ben Lomond. I still remember the view from the top: Loch Lomond lay blue and sparkling below, as smooth as glass. I could smell the fresh grass and taste the salt of my sweat on my upper lip, my legs burning from the climb. But more than that, I remember a feeling of triumph.
Family plays an important role in our development. We are not always cognizant of the wide-reaching impact our parents, siblings, and extended family have on us as we grow—for good or ill. So, in this essay, my family and their impact on me is my chosen subject. It’s difficult to sum up all of my feelings in just one article on my family, but I hope that I am able to do them some small amount of justice.
In an ideal world, everyone would have supportive, unconditionally loving families to hold them up and help them through life. Unfortunately, this is not the case. And this is why I feel so blessed to have grown up in the environment that I did.
When I was younger, everyone used to tell me how much I reminded them of my dad. At the time, it only provoked me; what growing girl wants to be told she reminds people of her stuffy, academic father? But, as time has gone on, I’ve realized what a compliment that is.
Most of my childhood memories of Dad are of him in his study. He is a professor and a historian, and even to this day, he always seems to have his head in a book. I was always a quiet kid, so he didn’t mind it when I sat with him while he read. His study had a window seat that looked over the garden, and I’d curl up there with a blanket and a book and keep myself busy.
We didn’t spend all of our time in silence. He’d tell me about his book and would encourage me to do the same, asking me about my favorite parts and why they stood out to me. More than ten years have passed since those days, and now I find myself with a Master’s in English Literature. I can’t help but think that I owe it all to him. Dad taught me to think for myself and showed me that knowledge is its own reward.
My mom couldn’t be more different from my dad. Where he is quiet and reserved, she is bubbly and extroverted. Where he prefers to stay at home with a good book, she likes to be out and about and gets antsy if she’s left sitting around for too long. Mom retired recently, but before that was a teacher. She complained about the long hours and pay, but she loved the kids she taught and gave them her all.
That’s what I’ve learned from her: if you’re going to do something, give it all you’ve got, even if it’s hard. Despite all their differences, that philosophy is one my parents share and one they impressed upon me from a young age. Even if you fail, so long as you can honestly say you tried, that’s all that matters. I’ll always be grateful to them for showing me that.
I feel lucky to have parents as supportive as mine, as I hope I’ve shown in this essay about our family.
For more essay examples and ideas on family related topics, check these pages:
- Childhood Years in Calamba
- The Power Of My Mother Tongue
- Describe Your Personality
- Family bond/relationships
- Become better human being
Now that we’ve given an example of a short essay about family, we’ll now show you how to simply sum up your family in ten sentences.
- I’m lucky to have a large family with whom I’m very close.
- My family composition includes twelve people besides myself: my grandparents, my parents, my aunt and uncle, my three cousins, and my older brother.
- My mother used to be an air hostess but retired a few years ago to help my father run their B&B.
- My aunt and uncle are both teachers at the same school where they have worked for almost ten years.
- I see both sets of grandparents regularly, as we often have them around for dinner or Sunday lunch.
- I sometimes play football with my brother and cousins in the fields by our house and it’s always a good time.
- For as long as I can remember, we’ve all gone away on an annual trip to a cabin in the mountains where we get to relax and get away from school and work.
- If I ever need assistance with something, no matter what it is, someone can always help.
- My family members love and support me, so I never feel lonely knowing that I have them around.
- I make sure that I never take my loved ones for granted and that I spend as much time with them all as I can.
Now that we’ve considered some tips and essay examples about family, let’s put together a checklist of essentials for writing an essay about your family:
- Do interview family members for more information regarding your lineage or important past events.
- Do brainstorm for ideas and memories you can write on. Dedicate a good portion of time to figure out what you can talk about that will support the theme of your essay.
- Do be honest. When writing a personal essay or memoir, it’s important to stay as honest as you can if you want to craft a meaningful paper.
- Don’t include random facts or bits of information just for the sake of padding out your paper.
- Don’t publicly publish a piece about your family without first having a conversation with them about it.
- Don’t forget to write with respect when you’re writing an essay on your family.
Frequently Asked Questions
Coming up with a strong theme for your essay will draw your readers in. You can also begin your piece with an interesting family story. Essay writing is about capturing the reader’s attention, so focus on saying something unique and interesting.
You may be wondering, “What should I include about my family in my creative writing?” Ultimately, it depends on what you’re comfortable sharing and what best suits the themes of your paper. If your work is going to be published, it would be wise to ask the involved parties for consent first, or at least run it past them.
You might be asking yourself, “How should I begin my article on my family?” Writing a compelling personal essay can be difficult, but you can begin by introducing your subjects. You should also make it clear in the first paragraph of your essay what your theme will be.
The length of your essay depends on what audience you’re writing it for. If you’re writing it for a class, your teacher will likely issue you a word count somewhere between 500 words - 1000 words .
User ratings:
User ratings is 4.5 stars.
4.5 /5 ( 9 Votes)

Creative Writer and Blog Editor
Despite my relatively young age, I am a professional writer with more than 14 years of experience. I studied journalism at the university, worked for media and digital agencies, and organized several events for ed-tech companies. Yet for the last 6 years, I've worked mainly in marketing. Here, at Studybay, my objective is to make sure all our texts are clear, informative, and engaging.
Add Your Comment
We are very interested to know your opinion
Thank you very much. Its great!
Love Angelina Grin and all her blog posts! Writing a family essay is hard but with this article, I took my basic knowledge of my first school and spoke about my world doubts and what I have a keen interest in.
Kity-porshel
I wrote an essay on my family titled Birthday Parties: How I'm a better person when my cousins visit. Thank you for the inspiration.
I spend quality time with my elder sister and parents, but I found that not everyone is able to write about a complete person easily. In my family essay, I wrote about house parties and what I'm proud of. I made my own based on your example.
Once I read the example, I knew I needed to ask for help. My family is a group of loving people who run a successful business together, but they're always busy. However, my cousins visit whenever my younger brother and I have birthday parties (uncommon occurrences??).
A family essay shows the importance of family and with these tips, I was able to talk about the professional lives of my grandparents and how my mum was a housewife.
Mindy in City
Thank you for the example it really helped. We weren't taught in school but were to write about someone asides from our nuclear family that teaches us values. I've never met an uncle, aunt, or cousin in my entire life.
It's hard to talk about my small and lovely family and everything they taught us. I wanted to write about my mother and father with love and respect, and this article helped me =) thanks!!
Thanks for this I made my own essay off the example. I'm an only child, and I love my family so much. I pray to God daily to become a better person like my parents
Helped with my wonderful family essay. They mean the whole world to me! They spent their entire life building a successful business and made me a better human being.
Mary-Annette
To avoid writing about a random group of people, I asked all my family members' permission; not everyone wanted in🥺.

Upgrade your writing skills!
Try our AI essay writer from Studybay today!
- Essay Editor
How Should I Go About Writing My Family Essay?: Examples and Tips

Family is an integral part of every individual's life. Delving into the intricate layers of family relationships and dynamics can yield a captivating essay. Here's a comprehensive guide with examples and tips to guide you through the process.
What Topics Should I Write About for My Family Essay?
Choosing the right topic is essential. Here are some suggestions:
Writing a Family Tree Dive into your roots! A family tree can be more than names and dates; it can narrate stories of ancestors, their challenges, achievements, and legacies. For instance, "When I looked into our family tree, I discovered that my great-grandfather was a sailor who traveled the world and had countless tales of adventures, some of which have become legendary bedtime stories in our family."
Describing My Family in My Essay Discuss each family member in detail. "My sister, with her fiery red hair and matching temper, is the exact opposite of my calm and analytical brother. Yet, when they come together, they create the most amazing music, with him on the piano and her singing."
Writing About a Personal Memory Share a poignant memory. "I remember the time when our cat, Whiskers, went missing. The entire family turned detectives overnight, searching for clues, putting up posters, and even setting up a 'cat trap' with her favorite treats. The adventure ended with Whiskers found sleeping peacefully in the neighbor's shed, unaware of the chaos she had caused."
Dos and Don’ts When Writing a Family Stories Essay
- Be authentic.
- Use vivid descriptions and dialogues.
- Respect privacy; ask permission if sharing personal details.
- Avoid making generalizations.
- Refrain from being overly negative or critical.
- Don't plagiarize; every family's story is unique.
Frequently Asked Questions
- What is a good hook for an essay on my family? As Tolstoy once said, 'All happy families are alike; each unhappy family is unhappy in its own way.' Our family, though, has found its unique shade of happiness.
- What should I include in an essay about me and my family? Descriptions of family members, memories, traditions, challenges, and lessons.
- How should I start an essay all about my family? Every time I think of the word 'home,' an image of our old cottage, Sunday dinners, and loud family debates comes to mind.
- How long should my essay about my family be? Length depends on the requirement; academic essays typically range from 500-1000 words, while personal essays can vary.
- How do I make my family essay engaging? Incorporate stories, memories, and emotions.
- Is it okay to discuss family challenges in my essay? Yes, but be sensitive and respectful.
- Can I add humor to my family essay? Yes, as long as it's in good taste.
Related articles
How to write about yourself: basic tips & examples.
Writing about yourself isn't always easy, but it is definitely an important skill to have. You might need to do this for a school application, a job, or just to understand yourself better. When you think about how to start an essay about yourself, it's good to consider what makes you special. What has happened in your life that's important to you? What do you care about? These questions can help you find the main parts of your story to share. Why Writing About Yourself Matters Writing about w ...
Rhetorical Analysis: A Comprehensive Guide
A rhetorical analysis essay is a part of the AP English Language and Composition exam. Due to its unorthodox purpose, rhetorical analysis can be hard to master at first. This article will help you understand what a rhetorical analysis essay is, learn about main rhetorical analysis strategies, and find out how to write a rhetorical analysis. What is a rhetorical analysis? As you can probably guess, a rhetorical analysis is a type of analytical essay. Alongside a synthesis essay and argument es ...
Effective Transition Words for Structured, Flowing Essays
Have you ever encountered an essay that flowed seamlessly, through a clear and logical path? That smooth flow is often achieved through the skillful use of connectors. Transition words, also identified as connectors, are the unrecognized heroes of succinct, cohesive writing, effortlessly leading attentive readers from one part to another. The correct usage of connectors also reflects the quality of your composition. In this instructional guide, let’s look at the importance of linking words, exam ...
3 Paragraph Essay: Structure and Writing Guide
There is a wide range of challenging and interesting writings in academic assignments. A 3 paragraph essay is highly rated in this list. What is the purpose of this project? What parts should be there? How to organize material correctly? These questions will be discussed in the article. The purpose of the 3 paragraph essay is to show a student's ability to fit a topic interpretation in a limited amount of words. This format is usually used for summaries, argumentative essays, and other papers, ...
How to Write a Good Conclusion: Outline and Examples
Writing a well-structured and insightful concluding paragraph is akin to putting the final cherry on top of a delicious cake – it completes the experience and leaves a lasting impression. Whether you are crafting a paper, a report, or research, creating a persuasive closing paragraph can significantly enhance your work’s influence. This guide delineates the specifics of how to write a conclusion, explores the essential elements of a closure, offers strategies for writing one that resonates, and ...
How to Write a Methodology in a Research Proposal
In academic research, crafting a solid methodology is crucial, acting as the foundation for a reliable study structure. It provides the framework that guides the investigation towards addressing research questions and achieving study objectives. Understanding ‘What is methodology in research?’, the components it entails, its efficient organization, and the essential steps required, is vital for aspiring academics. This comprehensive guide explores the intricacies of accurately generating a meth ...
A Guide to Writing a Great Short Essay
As a student, you're no stranger to the countless writing assignments your teachers toss your way. When you see that your next assignment is a short essay, you might think, "Oh, this will be easy!" I mean, it's only a few hundred words, right? How hard could it be? But here's the thing: writing a short essay can sometimes be even harder than writing a longer paper. So, let's work together and figure out how to make your short essays really stand out! The Basics of a Short Essay Format A short ...
How to Start an Essay with a Quote
Starting an essay with a quote is more challenging than picking some excellent words from a famous person. It's about finding words that make people want to read more. You may have tried before and ended up with something that didn't sound very serious. Don't worry; lots of people have this issue. This article will help you choose and use the best quote to begin your essay. Helpful Tips for Starting Your Essay with a Quote Using a quote at the start of your essay can get your reader's attenti ...

ADVERTISEMENT
9 Tips for Getting Started on Writing Your Family History
Sign up for the Family Tree Newsletter Plus, you’ll receive our 10 Essential Genealogy Research Forms PDF as a special thank you!
Get Your Free Genealogy Forms
" * " indicates required fields

Written by Diane Haddad, unless otherwise noted.
Once you’ve been doing genealogy research for a while, and you have a family tree or a computer hard drive or a filing cabinet with a bunch of notes and old records, you might wonder what to do with it all. Or perhaps you’ve always harbored the dream of sharing your family history, and you’re not sure how.
It’s a hard truth: Few people have much use for an unstructured assortment of documents and computer files. Even folks who are curious about their family history—and that describes most I’ve met—aren’t likely to sort through your research and rebuild the store of knowledge you’ve amassed over years.

If your family research is to live beyond you, you’ll need to do the work of putting it into some shareable, lasting form. That usually means summarizing your finds in writing, maybe enhanced with photos and images of interesting documents. Whether you go all-out with a self-published hardback or just pass out stapled pages at the next family reunion, you’ll create a legacy—a framework others can use to understand your family’s story and the genealogical evidence you’ve gathered.
We can’t promise the project will be a breeze, but we can promise it’ll be easier when you follow these tips and use our handy organizing worksheet.
1. Know Your Purpose
Before you begin, it’s important to know what you hope to accomplish with this writing project. Do you want to summarize all your research, share your family legacy, pass down the stories Grandpa told, tell how your family fits into local history, share the story of an ancestor or family you admire, celebrate your ethnic heritage, or something else?
A strong focus makes the project more manageable, says Sunny Jane Morton, author of Story of My Life . “A small, finished project is better than a three-volume tome that exists only in your dreams.”
Need help narrowing the scope? Morton advises looking at your research for the most compelling story or interesting person. Author Sophia Wilson, who penned an 160,000-word history of her family, started her project by writing as many family stories as she could think of, then turning them into short biographies of the people involved. She wrote every day for at least 15 minutes, but sometimes for hours at a time. Taken together, those biographies served as the starting point for her project.
Alternately, you could choose a topic that commemorates an upcoming family milestone, such as your parents’ 40th wedding anniversary. Or you might start with whatever is most doable.
Your audience is an important aspect of your goal. For a project just family will see, you might use a casual writing style, refer to relatives with familiar titles (“Great-grandpa Thornton”), and use in-text source information. If other genealogists will read your work in a newsletter, journal or published book, you’ll want a more authoritative style with an emphasis on your research process, and formal source citations in footnotes and source lists.
Think about your audience’s age (or level of maturity), too. Wilson recalls how her research turned up stories that might not be appropriate to a younger audience. “Instead of shifting the focus of my book, I decided that children could simply read the unvarnished truth once they were mature enough,” Wilson says. “Age-appropriate stories could be extracted and adapted for a younger audience, for whom I would also write at a lower reading level.”
“I kept coming back to what I wanted the project to accomplish (preserving and sharing memories for the younger generation) and letting that guide my decisions,” she says.
2. Make a Plan
An outline gives you a framework for building your project, especially if it involves multiple people or a long time span. Make a list of elements you want to include. Don’t worry about organizing the list yet.
Here’s an example for my maternal family history opus:
- a family tree of Mom’s family
- information about the places the family came from with a map, including why so many immigrated from each place
- names and immigration details of all the immigrant ancestors: Henry Seeger, Eduard Thoss, Mary Mairose, Thomas Frost, Edward Norris, Elizabeth Butler, Henry Hoernemann, Anna Maria Weyer, and so on.
- where these families settled in the United States, their jobs and their children
- Eduard Thoss tavern in Northern Kentucky
- info on Cincinnati Over-the-Rhine neighborhood, where so many settled
- Dierkes boys in family cemetery plot
- Henry Seeger’s cigar store, with photos and timeline, and two babies who died as infants
- Thomas Frost/Mary Wolking divorce
- Ade Thoss and the Covington Blue Sox
- possible family connection to Windthorst, Kan.
- death of Elizabeth Teipel Thoss and several of her children
- Benjamin Teipel trap-shooting invention and death
- Civil War service of Frank and Benjamin Thoss
- firefighter Raymond Norris and Newton Tea & Spice Co. Fire
- how Grandma and Grandpa met
Your list might cause you to rethink your project scope. For example, I’m seeing that I could divide up my project by family branches, breaking it down into smaller parts (and this is only part of my list).
When you know the topics you want to cover, arrange them in an order that makes sense to you. You could do chronological order, geographical order (group all information related to Germany, all immigration information, all second generation information), family branches one at a time, or some other arrangement. You could opt for a general overview then add several shorter profiles of specific ancestors or families.
Wilson shares how she thought about structure while planning her project:
One option would be maintaining individual biographies, organized in the book by birth year, generation or location. Or I could combine all biographies into a single narrative chronology, or even organize the stories by theme (women, farming, culture, etc.). I opted for the most straightforward and comprehensive order: chronological. With this approach, I gained a deeper understanding of how my ancestors’ lives developed over time, and how one event flowed into another.
Next, create an outline by organizing topics into sections or chapters. Read published family histories for examples. One of my favorites is Family by Ian Frazier.
3. Say It with Pictures
Pictures and graphs will engage your readers, help them follow complicated lineages and show what you’re talking about. “Plan as you go which pictures, documents, maps, charts and genealogical reports will best illustrate your narrative,” Morton advises.
Depending how many photos and documents you’ve found, you’ll want to winnow the options to those from key moments in your family history, selecting those that will reproduce well in the finished product. Consider adding transcriptions for hard-to-read or foreign-language documents.
Keep copyright in mind. If you plan to publish your work (including on a website), get permission from the copyright holder or owner of any images you didn’t create or that aren’t in your personal collection. For a quick read about understanding copyright laws, check out this article .
4. Get Organized and Utilize Apps
Now you’re ready to write. As you work, go over your records for families and people you’re writing about. Wilson developed a filing system that automatically sorted documents by individual. “I created a separate document for every event so I could easily insert new findings, titling each with the event, the date and the location,” she says. “I then grouped the documents into folders, one folder for each year.”
To help you organize source references, add in-text references with the title, author and page or record number in parentheses when you use information from a record, article, book or website. Also create a bibliography of sources as you go. This should include everything needed to find that source again: title, author, publisher or creator (such as the National Archives), publication date and place, website, etc.
Later, when your project is mostly complete, you can keep the in-text references, or number the references and create footnotes (short-form citations at the bottom of the page) or end notes (short-form citations at the end of a chapter). Include the bibliography at the end of your work. For help with source citations, use the book Evidence Explained by Elizabeth Shown Mills (Genealogical Publishing Co.).
You might have a writing head start if you can pull together blog posts or short essays you’ve already written about your family history. Your genealogy software or online tree might offer a timeline you can follow, or even generate a narrative report for you. For an ambitious project or if you do a lot of writing, you might invest in software such as Scrivener . Additionally, writing apps can help you create an outline, organize and edit your story.
Read: How to Create a Genealogy Source Citation
5. Generate Ideas through Prompts and Research
If you’re still having trouble knowing what to write, try answering the family history writing prompts in a book such as Stories From My Grandparent or from Family Tree Magazine . These will help you flesh out ideas and take your family stories in new directions.
Revisit your research for story ideas, and let what you find in documents inspire you. Wilson consulted books (both digital and physical) about her ancestors’ location and ethnic group, as well as documents on genealogy websites like Ancestry.com and Newspapers.com. One book on Ancestry.com contained all the church records for her ancestors, some written by her great-great-great-grandfather’s best friend.
Wilson also revisited local histories and newspapers she had found early in her project. “Now that I was further in my research, I recognized more names and better understood the relationships among them,” she says. “People I had dismissed as “townsfolk” turned out to be in-laws and close friends of my lineal ancestors.”
6. Seek Out Help
Look for writers’ groups and classes in your community. From online groups to friends and family members, having a community you can rely on for feedback and encouragement is essential.
Reaching out can also lead to new research finds, important for sourcing the details in your stories. Wilson connected with other family historians, as well as genealogical societies and libraries (who scanned entire chapters of reference books for her to consult). One cousin-in-law even sent her photos and a relevant family keepsake they found on eBay.
7. Begin in the Middle
Don’t let the “how to start” roadblock stall your project right out of the gate. If you don’t know how to begin, just start writing a story you like—maybe it’s about an ancestor’s immigration, military service or venture to the wrong side of the law. The words will flow from there.
“My goal wasn’t perfection, just to get memories on the page,” Wilson says about her first step of writing family biographies. “I didn’t waste time checking spelling and grammar—that would come later.” An interesting or dramatic event is often the best way to begin a story, anyway. Remember, you’re not carving in stone: You can always rearrange things later.
8. Write Naturally
If you’re writing for relatives, pretend you’re telling your family story to a friend. If you’re writing for a publication, tailor your work to that publication’s style.
Wilson had to wrestle with how to balance facts she found in her research with storytelling. “I thought of how much I hated history class growing up—all those names-places-dates to memorize, and no story to latch onto,” Wilson says. “I resolved to … strive for historical accuracy without resorting to the dry tone of a textbook.”
9. Take Your Time
A deadline can motivate you, but give yourself plenty of time. You want this project to add fulfillment to your family research, not cause stress. Start now and work on your writing project a little at a time, once a week or every evening if you can manage it. Imagine where you’ll be a year from now.
A version of this article appeared in the December 2018 issue of Family Tree Magazine , written by Diane Haddad. Sophia Wilson’s article on the steps she took to write her family history narrative appeared in the March/April 2022 issue of Family Tree Magazine .
Related Reads

Editors of Family Tree Magazine
related articles
Writing compelling characters in your family history.

Storytelling, Writing
7 creative writing forms for sharing your family history.

How to Create an Outline for Writing an Interesting Family History

Storytelling
How to share family history stories on the big genealogy websites.

Ancestry, FamilySearch, MyHeritage, Storytelling
- Skip to main content
- Skip to secondary menu
- Skip to primary sidebar
- Skip to footer
A Plus Topper
Improve your Grades
Family History Essay | How to Write? and 400 Words Essay on Family History
February 14, 2024 by Prasanna
Family History Essay: A family involves individuals living respectively that structure a gathering of people inside a local area. Individuals making this gathering are dependent upon connections either by birth or blood, and it involves at any rate two grown-ups as guardians and grandparents, along with little youngsters. The relatives have a common association between them. Thus, an exposition about family ancestry is a rundown of a person’s social personality and the equal relationship(s) he/she imparts to individuals living respectively.
Adapting family ancestry is indispensable to comprehend our economic well-being, mankind, and variety. History saves our recollections for ages to comprehend what their identity is and their geographic beginning. Having decent information on family foundation allows you to see the value in the things or penances made before by grandparents to encounter better things throughout everyday life. A person’s underlying foundations and beginning bring a self-appreciation revelation. Likewise, expounding on your family ancestry is one method of protecting its legacy for people in the future.
You can also find more Essay Writing articles on events, persons, sports, technology and many more.
How to Write a Family History Essay?
When composing a, there is a consistent construction you should continue in giving out your contentions. An appropriate diagram will deliver an energizing show of each segment, and it will interest the peruser. The standard design of an article has a presentation, body, and end. Here is a magnificent illustration of a layout for a family ancestry article:
- Topic: My Family History
- Introduction (Outline): Write a short brief about your family background and why your family is important
- Body: Write about your family members, how you live together and who your neighbors
- Conclusion: Rehashing your conflict, Sum up your key thoughts, and Give a last remark or reflection about the paper
Essay on Family History 400 Words in English
Would you need to know how everything began until here? My grandpa disclosed to me that he met my grandmother at a show where probably the best craftsman was performing during one of the late spring occasions in London. As he was moving alone, my grandpa moved toward a wonderful woman (who might turn into his perfect partner) to request that she dance together. They later consented to meet for a supper date. Our family lives in London. Without a doubt, this is the best family, and it’s an honor to be essential for it.
Each individual includes different sides inside his/her family; my fatherly side begins from Canada, while the maternal side is from America. Despite the fact that my extraordinary granddad comes from Spain, my grandpa and grandmother live in London. My granddad is Indo-British who functioned as a barkeep, no big surprise he adored shows! My dad fills in as a traditionalist for amphibian fauna while my mom works in the bread kitchen. My mom and father met in a store when they were both shopping.
Despite the fact that we live in a similar city, my grandparents have their loft, a separation from our own. We live as a group of five; father, mum, and three youngsters. As we as a whole live in a similar city, we (me and my two sisters) incidentally visit our grandparents during the end of the week to invest some energy with them; grandpa and I were doing some planting while my sisters and grandmother do cook and other house tasks. The connection between our extraordinary guardians and our own is extremely phenomenal.
At Christmas, every one of my youngsters, mum, and father travel to our grandparents for an entire week. During the new year, we get together at our home, my parent’s home, to invite the year as a whole family. Now and again during the end of the week, we normally invest the majority of our energy on the seashore swimming, besides on chapel days. As a family, our number one food is rotisserie fish, rice, and vegetables. In any case, my grandpa likes chicken hash.
All in all, the social conjunction between us is fantastic, which has made a powerful common bond for the family. From visiting one another, investing energy in the seashore, getting together suppers to usher in the new year, and observing Christmas as a family, the bond continues to develop. I’m favored to be essential for a particularly incredible family.

FAQ’s on Family History Essay
Question 1. Why is it important to know family history?
Answer: Knowing your family ancestry is vital. It empowers one to self-find himself inside the general public and like the heredity. At the point when you find out about your family’s past, you will comprehend the things you see and experience today. Composing an article on family ancestry requires a ton of comprehension and consideration regarding the viewpoints you need to depict. The basic factor being the family foundation, at that point seeing how you need to design and scribble down your thoughts.
Question 2. What are the points that can be mentioned in a family history essay?
Answer: You can write about family members, relations, values and traditions of your family. Write down the places from where your ancestors belong or the origin of your family. Also, mention the family reunion or gatherings or the occasions when you all get together.
Question 3. What family really means?
Answer: Family implies having somebody to adore you unequivocally disregarding you and your weaknesses. Family is cherishing and supporting each other in any event when it is difficult to do as such. It’s being the best individual you could be with the goal that you may motivate your adoration ones.
Question 4. Why do we need family?
Answer: Family is the absolute most significant impact on a youngster’s life. From their first snapshots of life, kids rely upon guardians and family to ensure them and accommodate their necessities. Kids flourish when guardians can effectively advance their positive development and improvement.
- Picture Dictionary
- English Speech
- English Slogans
- English Letter Writing
- English Essay Writing
- English Textbook Answers
- Types of Certificates
- ICSE Solutions
- Selina ICSE Solutions
- ML Aggarwal Solutions
- HSSLive Plus One
- HSSLive Plus Two
- Kerala SSLC
- Distance Education
How to Build a Family Tree
How to build a family tree: tracing your ancestors.
Your decision to start a family tree will take you on an interesting journey back through time. As a time traveler, your journey will begin with your life. Go back to your birth record and start to note the details of where you were born, the date, your parents full names, and be sure to include your mother’s maiden name. Next record details of places you have lived, your schooling, marriage, and children. Then begin to work back further and research your parents’ lives. (There is probably much about them that you don’t know.) Building a family tree can be a wonderful activity to share with your parents and grandparents—and if you are very lucky—a great-grandparent.
Your children or extended family may be interested now or in the future in researching their family tree, so be sure to record your findings carefully in a permanent place for everyone to enjoy long after you too have become an “ancestor.”
Linking generations, setting each in its unique historical perspective, brings them to life again for everyone.
Identify What You Know and Use Home Sources

- birth, baptismal, graduation, marriage, military, and occupational records
- death certificates, burial records, and obituaries
- yearbooks, newspaper articles, family letters, social activity mementos, sports awards, and other documents that might provide names, dates, and locations
Then look at your family’s religious records, old letters, photographs, and memorabilia. Print copies and label everything to document the source, and scan them when possible to save them digitally. Now you are well on your way to forming the branches of your family tree.
Next, contact family members and ask questions about their lives and those of other relatives. Interview all your oldest relatives first. Most of us later regret not doing that in time to learn from them. A sampling of questions might include the following:
- Where did they live?
- In what part of the country?
- What kind of dwelling did they live in?
- Did they move around while growing up?
- When and where were their relatives born?
- When did these relatives die, and where are they buried?
Take along some of your old photos and attic treasures to jog their memories. And be sure to ask if you may see their old family records, letters, photos, and memorabilia. These documents might help you expand your search. Take photographs of their mementos, records, and photos with your camera, phone, or bring a portable scanner. Document the photos you take with names, date, and place.
Listen to their family stories and make notes. Relatives often have different versions of the same story since each person remembers an event in his or her unique way, but these differences make it interesting! Share what you already know with them. Use a tape recorder or video camera if your relative feels comfortable with it—most mobile phones can make audio and/or video recordings today. Make your initial visits short with someone you are just getting to know. Always ask for permission first before you make copies and take photos, videos, or audio recordings.


Record and Document Your Information
After collecting family information, it is important to record it correctly on forms referred to as family group sheets and pedigree or ancestor charts (download a free fillable NGS Pedigree Chart and NGS Family Group Sheet ). Fillable forms let you type into them and save them digitally.
Be sure to indicate a source for each fact. Your goal is to document the details fully so you can pinpoint exactly where to find the records again. Then file the information in an organized way so that you can locate each individual in your ever-expanding collection. The best way might be to create a folder for each one (either on your computer or in your file cabinet) and include old photos of them, their families, homes, and cemetery markers, plus their important documents, letters, and memorabilia. Add their stories—both those you heard as a child and those family members tell you.
Two books can help you fully understand how to document your genealogy work:
- Mastering Genealogical Documentation , a NGS workbook by Dr. Thomas Jones, PhD, CG, CGL, FASG, FNGS, FUGA
- Evidence Explained by Elizabeth Shown Mills, CG, CGL, FASG, FNGS, FUGA
Prepare Yourself to Build a Strong Tree
The best way to start your family history and build a strong tree is to learn the basics of genealogical methodology.
- Purchase “how-to” books. One such book is the NGS publication Paths to Your Past: A Guide to Finding Your Ancestors, 2018 Edition . Within its pages, readers learn about research techniques and sources. A great starting place!
- Then more in-depth is the “how-to” book, The Researcher’s Guide to American Genealogy, 4th Edition, by Val D. Greenwood. It will be another great addition to your genealogy book collection. This is a comprehensive textbook with examples of case studies.
- If you are an NGS Member, please take the free course that comes with your membership called Family History Skills .
- Next, NGS members and non-members will benefit from enrolling in NGS’s Foundations in Family History education program, start with the Foundations 101 course and also consider the CGS course: Guide to Documentation and Source Citation course.
Decide What You Want to Learn
Pick an individual about whom your information is incomplete. For example, if you are missing information about one of your four grandparents, start with her or him. Try to obtain death, marriage, and birth records if available. Always work backward from the known to the unknown.
Step One: Vital Records Will Be Most Helpful

- divorce records
Most U.S. states have kept modern vital records since the beginning of the twentieth century. States that were part of the original thirteen colonies are the most likely to have pre-1880 vital records and church records available. Publications such as The International Vital Records Handbook , 7th Edition, and the booklet titled Where to Write for Vital Records provide records descriptions, addresses, and other helpful information. There is also a digital 2014 version available on the Slideshare website from the Division of Vital Records .
Do a Google search for websites for each state archives to learn more about accessing vital records in a particular state.
The FamilySearch Wiki also offers a state-by-state outline of where to find various records for each state. Enter the country, state, or county name in the “Search by place or topic” box or click on the map.
Church and religious records for baptisms and marriages are often substituted for civil vital records before civil vital records were uniformly collected. The best way to find religious records is to search in the county where the ancestor lived. Use a search engine like Google or WorldCat and use a search term with a county and state name, plus a religious denomination, as in “Methodist church and Franklin County, NY”. Also check with a library, genealogical, or historical society where your ancestor resided for advice on where to find historical records for the religious denomination of interest.
Census Records from 1940 back to 1790

- Ancestry (the free library edition, which contains census images, is available on site at many libraries and genealogical/historical societies, as well as at LDS Family History Centers)
- FamilySearch (free access from home once you sign up for a free account; all census images, innumerable other databases, and collaborative family trees)
- Findmypast (free at many libraries and LDS Family History Centers )
- MyHeritage (free library edition is available at some libraries and at all LDS Family History Centers)
- HeritageQuest (available at most libraries across the United States, many of which offer free digital access from home for many Ancestry databases, including census records, through your library card)
Census records can also be viewed on site at the National Archives and its branches .
State Census Records
Many states collected census information from their residents (and also what is called census substitutes) before 1790 or for particular years in-between decennial federal census surveys. The FamilySearch Wiki is a good source to consult for the full complement of records available, state-by-state.
The thirty-one Research in the States guidebooks from NGS also provide excellent record sources beyond federal censuses.
City Directories
City directories are directories that preceded telephone books, which were organized to find people and businesses . They arose from a need for businesses to contact customers, customers to find businesses, and for residents to find one another. Listings for individuals are organized alphabetically by surname and give a home residence and often an occupation, and place of business. Sometimes a listing will include the wife’s name and older children who may have been working.
City directories began to appear right after the American Revolution in larger cities and eventually spread to counties and towns. They were published yearly in most locations. By the mid-1930s they were discontinued in favor of telephone books and Yellow Pages. City directories are an excellent way to track the movements of people between census years and to separate people with the same name by using addresses and occupations as identifiers.
The best source for discovering early city directories is Dorothea Spear’s Bibliography of American Directories through 1860 . The Library of Congress has a full set of all copyrighted directories on microfilm or microfiche (and most directories are copyrighted). Internet Archive and the New York Public Library have been digitizing vast numbers of directories from microfilm, so check their websites for free access to digitized directories now online. Miriam J. Robbins’ free website Online Historical Directories is a growing compilation of online city directories throughout the United States.
The FamilySearch Library has a comprehensive collection, including pre-1860 directories—search the catalog by [STATE], [COUNTY], [TOWN] – DIRECTORIES or click on the state name at the bottom of their United States Directories page . Ancestry, Fold 3, and other genealogy subscription services have more limited but useful collections of city directory records. Libraries often subscribe to databases such as these and may offer additional electronic resources with city directories that are free for patrons. Consult a reference librarian locally for more resources available to you.
The Courthouse
Having collected the basics about your ancestors, you are now ready to visit or contact the courthouse in the locality where your ancestor(s) lived. Wills, probate, and land records are useful for adding information about an ancestor’s life and family relationships, especially pre-1850 when other records may not exist. Call ahead to find where the records are housed as many older records are moved to other repositories if a courthouse runs out of room. At the courthouse itself, in the town or county archives, or in a local library, you may discover:
- land records and deeds
- surveys and
- other records
The Handybook for Genealogists and Red Book: American State, County & Town Sources can help provide addresses.
If you cannot go to a courthouse in person, search the internet. Many town or county offices have digitized at least some of their records and made them available online. Check the local historical societies and the state archives to see if older records have been transferred there. Another option is to consult digitized microfilm of courthouse records on FamilySearch.org or see if a local FamilySearch Center still has microfilm for the needed county court records. You may also consider a visit to the FamilySearch Library in Salt Lake City (see below).
Library and Archives Research

NGS Book Loan Collection
If you cannot get to a genealogy collection or your library doesn’t have the book you want, ask if interlibrary loan (ILL) is available. The NGS Book Loan Collection , held by St. Louis (Missouri) County Library, offers interlibrary loan service to send books in the NGS collection to your local library, for your use. There are more than six thousand genealogies among the twenty thousand books in the collection, many of them circulating. This collection is open to everyone. If the book does not circulate, contact the library staff, they may be willing to copy specific information for your research needs.
Online Newspapers
Vintage and contemporary newspapers are being digitized continuously around the country. They can hold intimate details of our ancestors’ lives such as
- a birth announcement
- the story of a runaway bride
- a big family reunion
- the celebration of 50 years of wedded bliss
- a death notice or obituary
- trouble with the law
- community involvement or political roles
There are many free collections, starting with the Library of Congress newspaper collection, Chronicling America . Check Miriam J. Robbins’ state-by-state list of free United States Online Historical Newspapers . Look for local newspapers in the areas your ancestor lived. Many historical societies have preserved copies of early newspapers.
Subscription databases that offer online historical newspaper collections such as Ancestry, Newspapers.com, FindMyPast, Genealogy Bank, and others, might be available at no cost if your local library has a subscription.
Foreign-language newspapers can be particularly helpful because the obituaries they print often mention the village of origin of the deceased. These newspapers covered the communities they served more intimately, so obituaries tended to be far more expansive than those printed in English-language newspapers for the same person.
If a particular newspaper important to your family research has not been digitized yet, it may be worthwhile to seek out the microfilm or original print copies as an alternative.
FamilySearch Centers
The Church of Jesus Christ of Latter-day Saints has microfilmed
- vital, land, probate, tax, and military records;
- state and federal censuses;
- periodicals;
- family and local histories; and
- numerous special collections from all over the world
Many are housed in the FamilySearch Library (formerly the Family History Library) in Salt Lake City, Utah. Some of these vast holdings are available in digital form through the FamilySearch.org website and some on microfilm at the FamilySearch Library, or the more than five thousand FamilySearch Centers or Affiliates located throughout the United States and the world. Call your local center to get an idea of their holdings. The FamilySearch Library in Salt Lake City is worth the trip to access their full collections in one place. It is an accessible, easy to navigate city.
Genealogical Societies
Family history researchers should consider joining NGS and a local society.
NGS members receive outstanding publications and discounts on the following NGS items
- online store purchases
- research trips
- fees for the annual NGS Family History Conference
NGS members learn from
- how-to and methodology articles,
- online courses and resources,
- conference sessions, and
- social and digital media offerings
Another less tangible benefit of NGS membership is the camaraderie that our members experience with other like-minded family historians they meet through NGS—either through online educational courses, research trips, or in person at our yearly conferences.
Local society membership can be very helpful if they hold regular meetings with lectures and can give you guidance on local records. Consider joining a society for the area in which you are researching.
Learning More
At this point you have been working mostly on your own. You will probably benefit greatly from taking a more formal genealogy course.
NGS offers courses that provide you with the freedom to learn from home. The NGS Family History Skills online course—free to NGS members—is a good starting point for how to build a family tree. Next, investigate NGS’s building-block-study-program called Foundations in Family History , made up of three progressive parts:
- Foundations 101
- Foundations 102
- Foundations 103
With Continuing Genealogical Studies, NGS also offers courses on specific topics you will want to learn more about. The thirteen course topics include
- DNA and Genetic Genealogy
- land and deed records
- military records
- documenting your work and adding citations
- reading old handwriting and transcribing documents
Make sure you take time to go through the entire NGS Learning Center . You will find lots of details about our
- online courses,
- annual NGS Family History Conference,
- genealogy related books, and
- research trips.
You will also learn about our genealogy publications, including:
- the scholarly journal with case studies, the National Genealogical Society Quarterly
- NGS Magazine , which offers a wide variety of the most up-to-date topics and resources and
- NGS Monthly , a digital publication to help you learn about resources and methodology for research
And if you are looking for answers to questions or making connections with other genealogists, NGS offers FORUM , an online platform for its members. Its a great place to connect with others around the US and the world, share knowledge, and solve genealogical problems.
Also available are many, many Free Genealogy Resources . NGS has been building a repertoire of personalized learning tools so that everyone can learn in a way that suits them, and at every skill level.
NGS. Build Your Skills. Build Your Family Tree.
Sign up for our Upfront with NGS blog or our NGS Conference blog .
© 2018 National Genealogical Society. Complimentary articles are for personal use only and may not be copied or used for commercial purposes. All rights reserved and require written permission from NGS.
Welcome to the National Genealogical Society. Login or create a free account.

Who Counts as Family in a Family Tree? Who to Add and Who to Leave Out
Last Updated August 30, 2020
The term family tree is defined as “a diagram showing the relationships between people in several generations of a family.” Add your parents, grandparents and great grandparents and you’re well on your way to building your own tree.
But, as we all know, family is an incredibly complex concept with biological, legal, social and emotional elements. And, for this reason, the question of who counts as family in a family tree is far from simple.
In our daily lives, family often has less to do with biological or legal connections and more to do with personal relationships. Those people who are intimate parts of our lives, who we love and care for, who care for us, are our family. What makes a mother, father, sibling, child, grandchild is seldom straightforward.
But in a genealogical sense people often get muddled and are unsure who should be added to their family tree. Adoptions, step-parent relationships, unmarried partners, multiple marriages, the discovery that a parent or sibling is not related biologically – all of these scenarios may cause some serious head scratching.
And even if we don’t experience any of these instances in our immediate lives, most of us will encounter them as we dig deeper into our family’s past, leading us to ask:
“What constitutes family in a family tree?”
“Who should I add and who should I leave out?”
To answer these questions we have to ask ourselves another, “What is the purpose of a family tree?” Is it to lay out a biological map of our past, or to tell as accurate a story as possible about the lives of our ancestors?
There are very few who would argue that the purpose of genealogy is to simply understand the biological connections of humans. After all, family history researchers spend much of their time digging through old records and histories – social documents – trying to better understand the realities of those they are researching. This work makes it incredibly apparent that family is much more complex than a bloodline.
Yet most of us feel a need to create a tree that tells a biological story – a physical record of what we are made of in an attempt to understand our ancestors and ourselves.
But if family is more than biology, and it is family that shapes us, than shouldn’t our trees be more than biological record books? If we create a tree that reflects only physical relationships are we really building an accurate picture of our ancestors’ lives?
If we want to develop a full and accurate picture of our family’s past we need to document everything we can about the lives that created it – and that includes taking the time to discover and include non biological relationships. We need to tell the very complex story that is family , generation after generation, if we want to understand where we come from.
In a previous article we discussed the importance of adding non direct-line relatives to a family tree – such as aunts, uncles and cousins – to form a well-rounded family history. And this scenario is no different. Our trees should be filled with those people that our ancestors considered family – no matter their biological or legal relationship.
A first marriage of great grandmother Jeanie for instance – even if it didn’t produce any children – had a huge impact on her life, as did the unofficial stepfather of your grandfather. He may not be biologically or legally related but he surely influenced the kind of man your grandfather became and the lessons he passed on to you.
And adding these relationships to your tree will help you uncover new records about your family’s past as you branch out and create new pathways for discovery.
Of course, only you can decide who should appear in your own family tree – but when you do you should always take the time to properly document the relationships so that others know exactly what they are looking at .
A stepmother for instance, even if she is the only listed mother, should be labeled as such. This will ensure that future generations will have an accurate view of the past and other family historians will have the details they need to build on your research.
Almost every family tree program makes adding multiple spouses to a person and non biological relationships for a child possible. Look in the help documentation in whatever program you are using for help.
Here is a quick walk through for how to edit relationships and add more that one partner/spouse on Ancestry. Links to how to edit relationships on MyHeritage and RootsFinder are found below.
To edit relationships in an Ancestry tree simply view the profile of one of the people in the relationship. Now click on the Edit button in the upper right hand corner of the page and select Edit Relationships .

Once on the Edit Relationships screen you will see that each person has a dropdown box of relationship possibilities. Click on the box and select an option.
For a parent or child you can choose:
For a spouse/partner you have the option of:
On this screen you can also add additional partners and children quite easily, including adding a child from another marriage/relationship. To do this simply add a child and choose from parental options at the bottom of the screen.
- MyHeritage has several articles relating to this topic – including adding adopted children and partners – in their help center.
- RootsFinder information on editing relationships is here . Read our intro and how-to on using their free online tree here .
Also read: Are You Making the Direct-Line Mistake in Your Family Tree?
By Melanie Mayo-Laakso, Family History Daily Editor
Image: “Family of J. J. Moore. All but mother and two smallest children on steps work in Washington Cotton Mills, Fries Va. Smallest spinner (right hand end of front row) said she was 14, but she surely is not. The family came from a Carolina farm three years ago. Location: Fries, Virginia.” May, 1911. Library of Congress .
- 22,448 shares
12 thoughts on “Who Counts as Family in a Family Tree? Who to Add and Who to Leave Out”
> Why does an ex spouse of a childless marriage have to be included in a family tree?
A few reasons: First, as mentioned in the post, they may have influenced the next spouse that did have children. Second, it provides additional insight into where you can find records of your relative, e.g. where they got married might be where they lived. Third, records you find about this childless spouse might provide some clues about your relative. E.g, if you don’t know when and where that relative was born and you don’t know much about that from their parents or siblings, perhaps knowing when and where the childless spouse was born can provide a clue.
Of course it’s up to you whether or not to include that person. If you don’t have much info beyond just a name you _could_ just leave their name as a footnote somewhere. But that makes it harder to research your relative in case there actually are records with that person or if (gasp) that childless spouse did not end up being childless after all.
Why does an ex spouse of a childless marriage have to be included in a family tree? They have no bioligical connection to the family.My family wants to include this person and I’m very opposed !
Is my brothers wife’s children related to me.
You should be GRATEFUL your ex is willing to share family history with you! He doesn’t have to. How bitter can a person be?
I want to know what gives you the right to send my EX-HUSBAND all my personal family history. I am sick of him sending me things like a picture of my Grandparents graves, etc.. It is none of his business who is on my family tree! It is very intrusive to me and I am trying to find out if it is even legal!
In this case I list the parents under the birth notation giving their life span if available. ei Parents John William Jones [1891-1950] + Alice Smith [1895-1945]. Also note especially in small communities more than one offspring of the above parents could have married into the same blood-line.
In my experience living persons are marked as private listing no name – date of birth or any other info
Please respect the request of relatives to be left off to protect their privacy. I for one do not want my name and especially dob on anyone’s family tree.
List as much information as possible. Step’s, half’s, spouses and their families if discovered labeling with relationship. This practice has led me to “find” much information. Including, 2 boys and 1girl; the boys couldn’t be located when grandpa’s will was probated in the 1890’s. The practice has also led to many discoveries I have found no where else.
My advice is “always include” …you never know what discoveries the information will lead you to down the road.
We have many loving men in our family who have raised other mens’ children. This question came up every so often, especially as my husband adopted my children, and raised them from ages 1 and 4. I talked about their father in everyday conversations, both good and bad things, but after we split he stayed away so as not to confuse them. My children know their blood relatives, but have a closer relation with hubby’s family.
\We came up with this simple little rule that so far seems to make everyone happy: List the stepfather as “step” or “adoptive” or whatever, right along with the “bio” father. Do a full profile on both fathers. Both are important, as stated above.
Then think about your relationships with stepfather’s family, being sure to ask the children involved the tree is, after all, for them. Decide which step relatives have close relationships with your children: do they see each other at Thanksgiving, go on vacation together, friends on facebook, and so on. If the step relative is known, include them. If not, leave them off. They have their own tree if you want to look for further information. So on our tree, we included stepfather’s siblings and their families, parents, grandmothers and a few of his aunts and uncles. Each case is different, but the rule’s always the same, and it seem to cover what’s important.
I don’t add parents of a uncle/aunt by marriage because you are researching a whole different family then. I add all husbands, wives, children & stepchildren, but I only add siblings of my biological line & their spouses, children. It’s confusing enough without going off in other directions! One dna match of mine was adding the grandfather of his brothers wife!
It’s the old nurture or nature question that constantly comes up in psychology. It is all part of our story. For me, I’d rather study the complex, nuanced reality, than only consider the clinically biological.
Leave a Comment
Your email address will not be published. Required fields are marked *
Copy and paste this code: wuzopi *
Leave this field empty
Privacy Overview
The Human Family Tree Development Essay
- To find inspiration for your paper and overcome writer’s block
- As a source of information (ensure proper referencing)
- As a template for you assignment
The creation of a family tree is not only an entertaining activity that helps people find out their roots, establish connections, and observe a variety of genealogic lines. From a scientific point of all, all humans are the products of their family trees, and all primates usually share a common ancestor and possess diverged abilities (Mader and Windelspecht 654). The DNA inherent from ancestors defines certain physiological characteristics and body functions. Thus, the investigation of the existing lines of descent in a human family tree allows scientists to determine the worth of connection dots and differences and similarities between the ancestors.
Despite the intention to prove the progress and differences between the past and the present, certain connections remain inevitable and critical for understanding human evolution. A family or evolutionary tree represents a conventional structure that shows the relationships and documents common ancestry (Mader and Windelspecht 654). The purpose of any family tree is to demonstrate a lineage and enhance a better understanding of a crucial organizing principle of biological modifications. According to Mader and Windelspecht, Darwin’s idea that all humans evolved from apes is one of the “most unfortunate misconceptions” in the world (654). However, the dots in the human family tree reveal prosimians like lemurs and lorises as the first primates that diverge from the primate line, and apes, to which humans are related, represent the last group. This example proves that humans and apes might share a common ape-like ancestor, and humans cannot evolve from apes because both continue living at the same time. Therefore, connecting the dots in the evolutionary tree is important to avoid misunderstandings and wrong interpretations.
Sometimes, people do not find it necessary to know more about their ancestors, their existing differences, and their similarities. Still, there are many examples that explain the worth of such a connection. The evolutionary tree contains all lines of descent, and it is clear that the genes of the first two lineages are almost identical (Mader and Windelspecht 655). With time, genetic changes occur, and some of them are not related to adaptation. The split between humans and apes occurred about 7 million years ago in the human tree, and chimpanzees are the most closely related hominins that share about 90% of the human DNA (Mader and Windelspecht 655). This knowledge is important for such fields as psychology, medicine, and pharmacology because people might use these animals to promote new braincases and other experiments to help humans manage their health problems. Although many people reject the possibility of animal experiments for scientific purposes, the worth of the evolutionary tree in terms of finding the connections and biological similarities is evident.
In general, the reasons for connecting the dots of the human family tree and the awareness of human ancestors have to be clearly explained and recognized in biology. In addition to strengthening people’s understanding of the evolutionary modes, this knowledge helps explain the changes in human characteristics. It is important to find the answers to such questions as why evolution is not evident today or why human lines do not diverge the same way apes or other hominin representatives did. The human family tree is a vivid example of how to interpret molecular data and comprehend the split between human and ape lineages. Multiple benefits characterize the decision to connect the dots, and the most evident is the promotion of knowledge structuring in human evolution.
Mader, Sylvia, and Michael Windelspecht. Connect with LearnSmart Labs Online Access for Inquiry into Life . 16th ed. McGraw Hill, 2020.
- Streptococcus Pyogenes Overview
- The Genomics of Adaptation in Birds by Campagna & Toews
- Direct Estimation of Mutations in Great Apes Reconciles Phylogenetic Dating
- Unilineal Kinship Units
- Nonhuman Primate Conservation: Is It Possible?
- A Light Microscope: Function and Usage
- Disorders of Thyroid Gland vs. Normal Structure
- Menopause and Associated Anatomical Changes
- Cognitive Neuroscience: Methods and Studies
- Metabolic Responses to Exercise
- Chicago (A-D)
- Chicago (N-B)
IvyPanda. (2023, August 31). The Human Family Tree Development. https://ivypanda.com/essays/the-human-family-tree-development/
"The Human Family Tree Development." IvyPanda , 31 Aug. 2023, ivypanda.com/essays/the-human-family-tree-development/.
IvyPanda . (2023) 'The Human Family Tree Development'. 31 August.
IvyPanda . 2023. "The Human Family Tree Development." August 31, 2023. https://ivypanda.com/essays/the-human-family-tree-development/.
1. IvyPanda . "The Human Family Tree Development." August 31, 2023. https://ivypanda.com/essays/the-human-family-tree-development/.
Bibliography
IvyPanda . "The Human Family Tree Development." August 31, 2023. https://ivypanda.com/essays/the-human-family-tree-development/.
We use cookies to enhance our website for you. Proceed if you agree to this policy or learn more about it.
- Essay Database >
- Essays Examples >
- Essay Topics
Essays on Family Tree
12 samples on this topic
To some learners, crafting Family Tree papers comes easy; others need the help of various types. The WowEssays.com catalog includes professionally crafted sample essays on Family Tree and related issues. Most definitely, among all those Family Tree essay examples, you will find a paper that get in line with what you see as a worthy paper. You can be sure that virtually every Family Tree paper presented here can be used as a sharp example to follow in terms of general structure and composing different chapters of a paper – introduction, main body, or conclusion.
If, however, you have a hard time coming up with a solid Family Tree essay or don't have even a minute of extra time to browse our sample directory, our free essay writer service can still be of great help to you. The thing is, our experts can craft a sample Family Tree paper to your individual needs and particular requirements within the pre-set timespan. Buy college essays today!
Research Paper On Family Nursing
Ancestry: example essay by an expert writer to follow.
The Company
Example Of Essay About Political Science
Book" guests of the sheik" chapter 10-chapter 16 book review.
Book Review: Guests of the Sheik
Human Evolution And Tool Use Term Paper Samples
Essay on anthropology.
THE SCOPES TRIAL
Example Of Phylogenetic Family Tree Research Paper
Phylogenetic family tree report examples, morphology of the english language research paper examples.
Introduction
Report On A Tree Full Of Ancestors
Why so many people have problems with reading research paper.
Thesis Statement
Reading problems are common among children in their first levels of learning but it has been seen to continue in some cases up to adulthood. Many of the people with reading disabilities have been associated with limited intelligence and these people have at times been said to have autism. However, associating reading disorder with autism and limited intelligence is all wrong. This is because there is medical and academic proof that dissociates reading disorder with limited intelligence.
Brain Mapping
275 words = 1 page double-spaced

Password recovery email has been sent to [email protected]
Use your new password to log in
You are not register!
By clicking Register, you agree to our Terms of Service and that you have read our Privacy Policy .
Now you can download documents directly to your device!
Check your email! An email with your password has already been sent to you! Now you can download documents directly to your device.
or Use the QR code to Save this Paper to Your Phone
The sample is NOT original!
Short on a deadline?
Don't waste time. Get help with 11% off using code - GETWOWED
No, thanks! I'm fine with missing my deadline
Home — Essay Samples — Life — Family History — An Overview Of My Family History
An Overview of My Family History
- Categories: About Myself Family History Who Am I
About this sample

Words: 723 |
Updated: 1 December, 2023
Words: 723 | Pages: 2 | 4 min read
Works Cited
- The Holocaust Encyclopedia. (2022). United States Holocaust Memorial Museum. Retrieved from https://encyclopedia.ushmm.org/
- Protestantism. (2023). Encyclopedia Britannica. Retrieved from https://www.britannica.com/topic/Protestantism
- Janette Smith's Life Story: A Journey of Faith and Family. (n.d.). Personal memoir.
- Assembly of God. (n.d.). ReligionFacts. Retrieved from https://www.religionfacts.com/assembly-god
- The Woman's Hospital of Texas. (n.d.). Retrieved from https://www.texaschildrens.org/locations/womans-hospital-texas
- NASA's Space Shuttle Columbia Disaster: STS-107. (2023). NASA. Retrieved from https://www.nasa.gov/columbia/home/STS-107.html
- Hurricane Katrina. (n.d.). National Geographic. Retrieved from https://www.nationalgeographic.org/article/hurricane-katrina/
Video Version

Cite this Essay
Let us write you an essay from scratch
- 450+ experts on 30 subjects ready to help
- Custom essay delivered in as few as 3 hours
Get high-quality help

Verified writer
- Expert in: Life

+ 120 experts online
By clicking “Check Writers’ Offers”, you agree to our terms of service and privacy policy . We’ll occasionally send you promo and account related email
No need to pay just yet!
Related Essays
2 pages / 1039 words
1 pages / 507 words
4 pages / 1801 words
2 pages / 874 words
Remember! This is just a sample.
You can get your custom paper by one of our expert writers.
121 writers online

Still can’t find what you need?
Browse our vast selection of original essay samples, each expertly formatted and styled
Related Essays on Family History
McGoldrick, M., Gerson, R., & Shellenberger, S. (Eds.). (2014). Genograms: Assessment and Intervention. Routledge.Pedersen, P. B., & Draguns, J. G. (2001). Counseling across cultures (5th ed.). Sage Publications.Potts, M., & [...]
Understanding one's family cultural background is an essential aspect of self-awareness and identity. Family cultural background encompasses the traditions, beliefs, values, and practices that have been passed down through [...]
Family is an integral component of human life, offering both emotional and psychological support to its members. The significance of spending quality time with family cannot be overstated, as it fosters stronger bonds, promotes [...]
The family systems theory has a significant revelation on family relations. I firmly agree that to understand a particular family or a member, they should be around other family members. The emotional connection among different [...]
I was born in central Africa(Cameroon) in a small city called Bamenda a very rough and challenging community, an environment which the leaders are corrupt, fighting between the francophone and the Anglophone to stay [...]
Anderson, J., & Sabatelli, R. M. (2011). Family Interaction: A Multigenerational Developmental Perspective. Routledge.Bengtson, V. L., Acock, A. C., Allen, K. R., Dilworth-Anderson, P., & Klein, D. M. (2005). Sourcebook of [...]
Related Topics
By clicking “Send”, you agree to our Terms of service and Privacy statement . We will occasionally send you account related emails.
Where do you want us to send this sample?
By clicking “Continue”, you agree to our terms of service and privacy policy.
Be careful. This essay is not unique
This essay was donated by a student and is likely to have been used and submitted before
Download this Sample
Free samples may contain mistakes and not unique parts
Sorry, we could not paraphrase this essay. Our professional writers can rewrite it and get you a unique paper.
Please check your inbox.
We can write you a custom essay that will follow your exact instructions and meet the deadlines. Let's fix your grades together!
Get Your Personalized Essay in 3 Hours or Less!
We use cookies to personalyze your web-site experience. By continuing we’ll assume you board with our cookie policy .
- Instructions Followed To The Letter
- Deadlines Met At Every Stage
- Unique And Plagiarism Free
- About Project
- Testimonials
Business Management Ideas

Essay on My Family
List of essays on my family, essay on my family – short essay for kids in english (essay 1 – 250 words), essay on my family – for children (essay 2 – 300 words), essay on my family – paragraph (essay 3 – 400 words), essay on my family –topics (essay 4 – 500 words), essay on my family (essay 5 – 500 words), essay on my family – why i love my family (essay 6 – 500 words), essay on my family – for school students (class 4, 5, 6, 7 and 8 standard) (essay 7 – 500 words), essay on my family (essay 8 – 750 words), essay on my family – long essay (essay 9 – 1000 words).
A family is one of the greatest gift god has given to all living creatures on the earth including humans. It is a privilege to have a happy family as not everyone in the world has it.
The joy of living with your parents, fighting with your siblings over petty can just make you smile the moment you think of it. In order to inculcate the values of a family in the students, we have composed some short essays for students.
These essays are suited for students of all ages and classes. Not only these essays shall give an insight on how a family should be but shall also enrich the students with the moral values of a family.
Audience: The below given essays are exclusively written for kids, children and school students.
Family is important to every one of us and we all love our family. Wherever we go in this world and whatever we may achieve, our heart and soul will always be in our home because it is where our beautiful family is. Nothing in this world can be stronger than the bonding of the blood . The members of the same family may have differences of opinions, may quarrel often for silly things but in spite of all these it is our family that supports us during our ups and downs.
As the saying goes, “ Family is the best thing you could ever wish for. They are there for you during the ups and downs and love you no matter what”.
Contrary to this saying, we cannot choose our family as we choose our friends. But I can say that I’m blessed with a wonderful family. My family is very small with four members – my mother, my father, my elder sister and me. My family is a middle class family and my father is officially the bread winner of our family. My mother supports him financially by taking tuitions for school children.
We do not have much money or wealth but what my family has in abundance is love for each other which cannot be replaced by anything else in this world. My father and my mother are the role models to my sister and me. They struggle a lot to give us a better life. More than anything they have taught us discipline and morals of life which is helping us to lead our lives in a righteous path even today.
I cannot ask anything more to God since he has already showered me with my family which I treasure the most every second and will safeguard even in the future.
The family is a valuable god gift which plays a most crucial role in every individual’s life. I love my family very much because all of my family members stand in my good as well as bad times. From moral teachings to love and support, my family has always helped me without any demand. There is no doubt that we experience our biggest triumphs when we really connect to them.
My family is like a strong pillar for me, on which I can rely blindly anytime I require support. From my family, I have learned the social graces of loyalty & cooperation.
My family consists of my grandfather, my grandmother, my mother, my father, two young sisters and myself. My grandparents are the pillars of my family and my grandfather is the head of my family. He is the one whose decision relating to any matter is final and all of us do respect it.
Right from my childhood, my family members have prepared me for the challenges that I’ll face in the years ahead. In addition to this, all of my family members help and serve each other at times of need. These qualities that I have learnt from my family has helped me to shape my adult life in a right manner.
I am really very attached to my grandfather. He holds an excellent life experience because he has already faced so many ups and downs. My Grandfather has helped me to build my perception & vision towards society.
My family has always been there to motivate and encourage me to overcome all difficulties in life and achieve success. The role of every member in my family is unique and important in their own way. I thank God that I have grown up in a family full of love and discipline. My family values will definitely help me in becoming a better person.
A person without family and its love never becomes completely happy in his/her life. I am complete and happy with my family that includes five members. My family is a group of five including me, father, mother, brother, and sister. Family bonding is a unique type of love that gives you every lesson needed to live a harmonious life.
Growing under the supervision of a caring and loving family will increase our social values and overall well-being. Each member of my family carries out equal responsibility in sculpting the strong bonding needed for a better future and develop moral importance in each other.
My father owns a successful business of office stationery store. He uses the money to cover all our expenses and give a better lifestyle to the family. He works hard day and night to get us better education, food, home, etc. He hides all his tiredness when he comes home after a long day to spend quality time with us.
My mother is a talented homemaker who also does a part-time tailoring at home. She does all her duties with at most interest, from taking care of us to all the household chores and finds time to pursue her passion as well. She is a multi-tasker and does all the tasks from helping us in our studies to preparing delicious healthy foods to sculpt us into a better human being.
My brother is an engineering graduate and does a job in a well-known company. He is my best well-wisher and helps me in all ups and downs. My sister is also an engineering graduate and an employee in an IT company. She always finds time to help me with all my difficulties and she is my secret keeper too.
My family is a lifeline to whom I can run to, whatever may be the situation I am facing. My family guides me to be a good person and help me in nurturing good values. We, humans, are animals that live together spreading love and care for each other, and this togetherness is called family. The absence of such a divine bonding make us equal to animals.
Family value and growing in such a caring surrounding helps me to pass all the struggles and hardships that I face in my daily life. Whatever be the situation we are facing, our family will never leave us alone. My family is a blessing for me and I value everyone in my family with equal respect and love.
Most of the people in the world are blessed with having a family. A family, with whom you can share all your joys and sorrows, who is there to guide you through your growing years, who stands by you in the toughest of the situations. I too am blessed to have such a family.
My family is one the most bizarre family in the world. We are four people, my mother, my father, my younger brother and me. While my father is the one who does work for a living, it is my mother who is the boss of the house. My father is a humble person. He is an officer in a government department. My mother is a housewife. It is our mother who takes care of our studies as our father is often busy with his official assignments and even travels for days together. We just miss him when he is not at home.
He never scolds us. But, our mother is just the opposite. She wants us to remain disciplined and we often get scolded by her. However, our father comes to our rescue most of the times. My brother, still in school is the one with whom I love to spend my time the most. Not because I love to play with him, but because, being the elder sister, I enjoy instructing him and showing him who is more powerful at home. He, at a time, seems so helpless when our mother says to obey his sister. I just love that moment. But not all days are the same. I hate having to study all along while he gets to play more than me.
The Atmosphere in my Family:
We largely have a peaceful atmosphere at home. After school, our time is spent on studying, playing and watching television, which of course our mother does not like. Unlike other couples, my mother and father seldom have a fight. In fact, as soon we see an argument brewing up, one of them just withdraws and it is just rare to see a heated conversation between them. This is what I like the most about them as I feel that my parents are so cool. It is only me and brother who love to fight with each other.
However, we know that behind those fights, it is actually our love for each other which binds us together. I just enjoy being at home spending time with my parents and my brother. I just feel how bad it would be when tomorrow I and my brother shall move on for our professional lives and we shall not be able to spend much time together. However, it is the memories of today which shall be with me forever and will bring a smile on my face anytime when I feel low.
The Importance of a Family:
A family is said to be the first school of a child. It is from here you start to learn how to speak, walk and interact with the world. It is important to value the importance of a family in one’s life. At times, people feel that they are grown-ups and that their parent’s advice does not matter anymore, but that is not true. It is the elders of the family who at any given of time would know the world better than us and we should all respect our family members and love our siblings as well. It is the family who builds our character and we should feel fortunate to have a family around us.
Introduction
My family values are what I take so dear to my heart because they have made me what I am today and I plan on passing these great values to my children in future. Every family has those things, acts and values that they hold in high esteem and they cherish so much. These vales have become a part of them: most times, it is what distinguishes the traits in each family and in some ways it makes or mars the future of the family members. Same applies to my family, we have some set values that has become a part of us and it has made my life a lot better because I have become a better person who is not only valuable to himself but also to the society at large. I will be sharing some of these values with you.
My Family Values:
Some of my family values include:
1. Honesty:
This is a principle that is highly protected in my family. My dad has this saying that, “honesty is the best policy.” Ever since I was little, my family has taught me how to be honest and the benefits that lie within. Sometimes, my parents even test us in ways we were not expecting and a reward is given to the person that comes out honest. This is one of my family values that I cherish so much and I am proud that it is what my family hold in high esteem.
2. Kindness to Others:
This is not a common trait to all. My mom has this belief that if the world and everybody in it shows love and kindness to one another, there will be no hatred and wars will be eradicated. This is a family value that we cherish so much. I learnt to show love to everybody. Even when we did not have much, my parents will still give to those who are needy. My dad says that the world is like a river, we would eventually flow into one another later and you do not know the future, the person you helped today might eventually be of help to you tomorrow.
3. Education:
This is a value that has been passed from generation to generation in my family. My dad would say that education is the best legacy you can give to a child. My family does everything in their capacity for you to get a sound and benefitting education. The acquisition of knowledge is also quite important. All of us try to gain more and more knowledge because we all have a family slogan that says “knowledge is power and that power makes me a hero.”
4. Dress and Appearance:
This is a religious value we cherish in my family. My dad would say that you are addressed the way you dress. I do not want to be address wrongly and give out a wrong impression. So, our appearance really matter a lot to us and the way we dress.
Conclusion:
Every family has one thing or the other that they hold in high esteem and tend to pass on from generation to generation. This is what makes a family a united sect not because we are related by blood but because of we share the same values.
Introduction:
Why I love my family is a question that has been floating through my mind for a very long time because no matter how hard I try to pin out a reason why I love them, I just can’t find one. This can be due to fact that they mean the whole world to me and I will do anything for them. I love my family a lot and I would like to share some of the reasons why I love my family and will never trade them for anything.
Why I Love My Family:
I have a family that consists of 6 people: my father, my mother and four children which includes me. For you to understand why I love my family I will tell you a little about each of them and why I love them so much.
My father is the best father in the world: well, that’s what I say. He is a business manager. I look up to my father a lot because I will like to take a lot of his behaviours and make it mine. He taught me to be contented with whatever I have. We did not have much when I was growing up; my dad lost his job and still did not allow anything of the pressure change how he behaved to us at home. He is caring, gentle, accommodating and disciplined.
My mum is the best cook in the world. I do not know where I would be today without my mum. I owe her a lot. She is a teacher by profession and this fascinates me a lot because not only is she inculcating knowledge in the young minds of tomorrow, she is also building the future of our society at large. I want to be like my mum. I remember those times when she had to sacrifice when the most precious of her things just to make me happy. She is loving, caring, understanding, accommodating. In fact, she is everything you can ever wish for in a mother.
My elder sisters are the best. Although they can be frustrating sometimes but that is mostly because of my stubbornness. They pretend they do not really care but deep inside they do. The things they do even subconsciously say otherwise. I remember a day in elementary school, I was being bullied a boy in class. On this particular day, he hit me. Unknowing to me, my sister heard about it and she beat the boy and made him apologise to me, I felt so happy that day because I had someone who had my back.
My brother is one of the best gifts I have received. He is the last child and this gives him an opportunity to be annoying if you know what I mean. He is joyful and always ready to heed correction. There was this day, I heard him bragging to his friends about how awesome I am, and I was the happiest that day.
We all have one reason or the other on why we love our family. I love mine because they are the best gift I could ever ask for and the fact that they have been there for me through the good, bad and funny times.
Importance of family is something that is greatly overlooked and underrated in the world we live in today. The definition that the family had about one hundred years before now was very clear. Back then, a family was believed to be a unit that consisted of the father that was in charge of the finances of the family, a mother whose primary duty was to look after the home and take care of the children and then there were the children. Largely based on the region you are from, a family can also include members of the extended family like aunts, uncles and grandparents. This type of family system is referred to as joint family.
Family Importance:
A family that is important is one that is very strong. If a family is going to be very strong, there is a need for the bond between them to be very strong. Bonds that help in keeping the members of a family with each other are relationships. If there are very strong relationships among all the members of a family, there is going to be stronger commitment between all of them and the family as a unit will be very important.
Better communication is also a result of family relationships that are very strong. If all the family members can take time out to talk and know each other well, the bond between them is bound to be very strong. Even if the conversations are about big things or small things, it does not really matter. The most important thing is that all family members stay connected to one another. It is very important that they all list to each other and understand every member.
How to make Family Bonds Very Strong:
We have various things that can help our family bond to improve.
A few of them include:
1. Love: love is the most important thing we need for our bonds as a family to improve. When we love the members in our family, we will also be able to know all about privacy, intimacy, caring, belonging and sharing. When there is love in a family, the family will prosper.
2. Loyalty: loyalty is something that comes as a result of love. Family members should stay devoted to each other. It is important that we are able to count on our family to have our back anytime we are facing problems.
The importance of family can never be overstated even though we live in a different time now and our attitudes to relationships, marriage and what a family should be has changed. The family is something that we need to help share our problems and be there for us anytime we have issues. A lot of the things that were not acceptable in the past and we now see as normal. Even with all the changes that the society has effected on our family system, the family still remains the major foundation of our society and this will remain the same.
My family is the best gift I have got. A family can be simply said to mean a social group of different people in our society that includes one or more parents and also their children. In a family, every member of the family commits to other members of the family in a mutual relationship. A family is a very important unit and the smallest unit in the society. A family whether a big one or a small one is of very great importance and use to all of its members and is believed to be the unit of our society that is strongest because the society is formed from the coming together and culmination of various families.
In many cultures, the family serves a child’s first school where the child learns all about their traditions and cultures more importantly learn about all the rudimentary values in life. A family is very essential in the teaching of healthy habits and good manners to all the members of the family. It gives the members of the family the opportunity to become people with better character in our society. I feel very lucky to be born into a small and lovely family; I learnt a lot of things from my family.
I am from a middle class and average family with six members (my father, my mother, my grandmother, my grandfather, my younger brother and me). My grandfather is the head of the family and we all respect and listen to him. He is really wise and tries to advise each and every one of us using his many life experiences. He has been involved in many interesting and adventurous activities that he tells me about all the time. Most of the time, he has the final say on all of our family issues and he does his best to make all his decisions impartial.
Any time we are eating today as a family, he sits at the top of the table; we all have designated seats at the dining table. When my brother and I are available, my grandfather teaches us about our traditions and cultures. My grandfather is very friendly and has a cool and great personality and tries to talk nicely and calmly to everyone passing across his message without being rude. He helps my brother and sometimes me with our assignments. He majorly teaches us about all of the tools we need to be successful in life including punctuality, discipline, moral, cleanliness, continuity, honesty, hard work and trustworthiness.
My lovely grandmother is one of the nicest people I know, she tells my brother and I lovely stories every night. My father is a civil engineer and he is very hardworking, sincere and punctual. He is the breadwinner of the family and does his best to provide for every member of the family even if that means he has to work extra hours. My mother is very sweet and takes care of every member of the family even though she works as an accountant at a firm. She wakes up very early in the morning to make preparations for the day. My brother is a funny and jovial person that enjoys sporting activities and I love him so much.
Sometimes I wish my cousins, uncles and aunts lived with us, I love having them around. There are a lot of advantages and disadvantages of having everyone around. I have highlighted some below.
Some advantages are:
1. It gives a better routine of living that can contribute to a proper growth.
2. Having a joint family helps in following the numerous principles of an equitable economy and helps teach discipline and respect. It also teaches us how to share the burden of other family members.
3. There is the understanding of having to adjust to the needs of other family members.
4. The children in a large family get to grow up in a happy environment because they have children of their age around that they can play with.
5. All the members of a joint family are usually very disciplined and responsible as everyone has to follow the instructions of the family head.
Some of the disadvantages include:
1. There is always the chance of a rift or fight between the family members because of the possible imbalance of feelings of oneness, brotherly love and feeling of generosity.
2. There is a chance of the members of the family that earn very high looking down on members of the family that do not.
The concept of family is important in India for every individual. Family defines an individual background in terms of social relations and growth. Families influence the lives of individuals from childhood to adulthood especially in decisions concerning life milestones like marriage and career paths. Indian families live together for up to four generations under one roof and they manage to maintain lose family relations compared to other families across the globe. Indian families tend to stick to their cultural practices as a family and they maintain religious practices that cut across the family. Elders in Indian families are respected by the members of the family and their opinions are considered during decision making.
What Family Really Means :
Basic knowledge defines a family as a group of people who share genetic and legal bonds. However, the concept of family means a lot more for other people than just the bond and it incorporates the concepts of culture and religion. In India, the concept of family differs from what the rest of the world perceives as family.
Families in India go beyond nuclear and extend to wider circles, whereby the extended family lives together and are closely related. The relationships in the family are strong such that cousins are considered siblings and aunts and uncles are considered parents. Family also means the unconditional love among the members of the family whereby there is support in terms of finances and emotions.
Why the Family is so important:
The family plays a central role in lives of individuals in teaching of moral values. Parents, aunts, uncles and grandparents have been known to teach the children on morality and disciplinary issue s in most cultures. Both spiritual and moral values are instilled through family. Family give a sense of belonging to individuals because they are over by the family and supported at all times.
A family will always support its members with needs including financial and emotional needs. In a family, there has been established levels of satisfaction and happiness from the joy of being together. Families also helping community development through contributions and participating in activities in the community. The family is important in the society in maintaining order, discipline and peace.
I come from a big family. My family has not moved to an urban area and so we still live as a wider circle together with the extended family. In my nuclear family, I am the first born of four children. I have one sister and two brothers who are still at school. I have three aunts and two uncles. My cousins are twelve in number and most of them are at school except for the youngest ones.
My grandparents are very old and they do not get out of the house much and are being taken care by my parents and aunts. Most of the children are always at school and the house gets quiet but during holiday, we all unite together as a full house. My family is of the middle class in terms of wealth. Our religion is Hindu and we all practice the Indian cultures and traditions. What I love about my family is that everyone is a good cook and the food is always amazing. Members of my family are kind and respectful and that is why we rarely have disputes. The family support is strong and we all love each other.
Why I love My Family:
Having a big family is interesting because the house always feels warm. As I had earlier mentioned, my family is made of good cooks, which makes me love them. There is always teamwork within the family and good relationships are maintained. I like the adventurous nature of my family because we always have fun whenever we go for holiday vacations or have a family event.
Moral cultural and spiritual values are highly cared for in the society. My family is oriented in good moral values and believe we make a good role model for the society. Despite the influence of education, the family has been able to maintain the culture and traditions of Indian people. The love that exists in my family is precious and that is the most important value of all times because what family without love?
Our Weekend Outings and House Parties:
We do not have many of these in our family because of the different schedules among the members. We only have weekend outings and house parties during holidays. Birthday parties are and weddings are the parties that we frequently have as a family. I love parties at home because the food is usually exceptionally good. Also, the dancing and happy faces. Weekend outings are usually in form of picnics and they are usually full of games.
Cousins Visit during Summer:
My family is young and only three of my cousins are in college. The rest are in high school or elementary schools. Whenever my cousins come home from school, it is a happy moment for the whole family and we host parties to welcome them home. Whenever my older cousins are at home, I enjoy their company and I love to hear stories about college because that is where I will be in a few years’ time.
In the spirit of holidays, we have a vacation or two in a year. During these vacations, plans begin early and when the time comes, it is enjoyable and relaxing. Vacations for us as children tend to be more enjoyable because we have an environment away from home and with minimal parental supervision and we tend to explore and talk among ourselves. Team building during vacations strengthens the bond in families.
Family is a blessing to individuals because that is where they belong and it is what defines them. A good family is built through moral values and team effort. Having family events and parties or vacations re important is strengthening the relationships within a family. A happy individual is definitely from a happy family.
Family , My Family , Relationships
Get FREE Work-at-Home Job Leads Delivered Weekly!

Join more than 50,000 subscribers receiving regular updates! Plus, get a FREE copy of How to Make Money Blogging!
Message from Sophia!
Like this post? Don’t forget to share it!
Here are a few recommended articles for you to read next:
- Essay on My School
- Essay on Solar Energy
- Essay on Biodiversity
- Essay on Globalisation
No comments yet.
Leave a reply click here to cancel reply..
You must be logged in to post a comment.
Billionaires
- Donald Trump
- Warren Buffett
- Email Address
- Free Stock Photos
- Keyword Research Tools
- URL Shortener Tools
- WordPress Theme
Book Summaries
- How To Win Friends
- Rich Dad Poor Dad
- The Code of the Extraordinary Mind
- The Luck Factor
- The Millionaire Fastlane
- The ONE Thing
- Think and Grow Rich
- 100 Million Dollar Business
- Business Ideas
Digital Marketing
- Mobile Addiction
- Social Media Addiction
- Computer Addiction
- Drug Addiction
- Internet Addiction
- TV Addiction
- Healthy Habits
- Morning Rituals
- Wake up Early
- Cholesterol
- Reducing Cholesterol
- Fat Loss Diet Plan
- Reducing Hair Fall
- Sleep Apnea
- Weight Loss
Internet Marketing
- Email Marketing
Law of Attraction
- Subconscious Mind
- Vision Board
- Visualization
Law of Vibration
- Professional Life
Motivational Speakers
- Bob Proctor
- Robert Kiyosaki
- Vivek Bindra
- Inner Peace
Productivity
- Not To-do List
- Project Management Software
- Negative Energies
Relationship
- Getting Back Your Ex
Self-help 21 and 14 Days Course
Self-improvement.
- Body Language
- Complainers
- Emotional Intelligence
- Personality
Social Media
- Project Management
- Anik Singal
- Baba Ramdev
- Dwayne Johnson
- Jackie Chan
- Leonardo DiCaprio
- Narendra Modi
- Nikola Tesla
- Sachin Tendulkar
- Sandeep Maheshwari
- Shaqir Hussyin
Website Development
Wisdom post, worlds most.
- Expensive Cars
Our Portals: Gulf Canada USA Italy Gulf UK
Privacy Overview
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
Tree Essay for Students and Children
500+ words essay on tree.
Tree Essay- Trees are our best friends because they clean the air we breathe. Likewise, they also clean the water and soil and ultimately make the earth a better place. It is also a fact that people who live near trees are healthier, fit, and happier than people who do not.
Moreover, it is our responsibility to look after our friends who serve us in many ways. Most importantly by saving plants, we are not doing any favor to plants but to ourselves only. Because trees and plants life does not depend on us but our lives depend on them.

Importance of Trees
Trees are important to us in a lot of ways and we cannot ignore their importance. They are important because they give us fresh air to breathe , food to eat and shelter/shade from sunlight and rainfall . Besides this, there are many medicines in the market that are made up of trees extracts. Apart from this, there are plants and trees that have medicinal value.
They bring peacefulness; create a pleasing and relaxing environment. Also, they help in reflecting the harmful rays of the sun and maintaining a balanced temperature . Besides, they also help in water conservation and preventing soil erosion . They also manage the ecosystem and from ancient times several varieties of plants are worshipped.
Get the huge list of more than 500 Essay Topics and Ideas
Benefits of Trees
Trees provide us many benefits some of which we can’t see but they make a huge difference. They help in fighting back the climate changes by absorbing greenhouse gases which are the main cause of climate change.
Moreover, they replenish groundwater and filter the air from harmful pollutants and odors. Besides, they are a great source of food and the king of fruits ‘Mango’ also grow on trees.

Moreover, they are the cause of rainfall as they attract clouds towards the surface and make them rain. They can be teachers, playmates and a great example of unity in diversity.
Above all, they are a good source of reducing air, water, and noise pollution.
Value of Trees
When a seed of a plant or tree grow it makes the area around it greener. Also, it supports many life forms. Birds make their nests, many reptiles and animals live on it or near it.
Besides, all these many beautiful flowers, food growing on it. Moreover, many parts of trees such as roots, leaves , stem, flower , seeds , are also edible. Most importantly they never ask anything in return for their services and the gifts they give. Trees also keep the balance in the ecosystem and ecology.
To conclude, we can say that trees are very important and beneficial for every life form on earth. Without them, the survival of life on earth will become difficult and after some time every species starts to die because of lack of oxygen on the planet. So, to save our lives and to survive we have to learn the importance of trees and also have to teach our children the importance of trees.
Customize your course in 30 seconds
Which class are you in.

- Travelling Essay
- Picnic Essay
- Our Country Essay
- My Parents Essay
- Essay on Favourite Personality
- Essay on Memorable Day of My Life
- Essay on Knowledge is Power
- Essay on Gurpurab
- Essay on My Favourite Season
- Essay on Types of Sports
Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *
Download the App


IMAGES
VIDEO
COMMENTS
A family tree is a representation of the lineages of a particular family mainly consisting of relatives stretching as far as possibly establishable by the family. A simple family tree would basically constitute of great grand parents, grand parents, parents, siblings, cousins and so on. Get a custom essay on Family Tree and Its Importance.
Family trees are a fascinating way to explore the history and connections within a family. They provide a visual representation of the relationships and lineage that have shaped an individual's identity. In this essay, we will explore the significance of family trees and their impact on personal identity and understanding of one's heritage.
A family essay takes a close look at the bonds and experiences within families. It's a common academic assignment, especially in subjects like sociology, psychology, and literature. ... For starters, begin with mapping out your family tree. Ask your family members for help and go as back in time as possible. Essay writing is a time-consuming ...
Examples Of Family Tree Essay. Family Tree While I know a lot about my family background on my mother's side, I know a lot less about my family background on my father's side. My father does not have an extensive knowledge of his family history and can be less than candid about his family background. I do know that my relatives on both ...
Essay about family tree - Research essay. Introduction. In my research paper, I have studied my family tree and have turned up information about people in my family. This information includes things that appear to define them or their character today and/or in the past. Thelma Griffin: mother of Peter Griffin. The line starts with Thelma Griffin.
Family histories can be one of the more creative forms of genealogical writing, as you can include all of the interesting facts about an ancestor's life. The researcher's methodology and analysis is not usually included in a family history- the writing should only focus on the family/ancestor. Family histories are a great way to preserve ...
Bliss! "Like a tree, a family is born, flourishes, branches out, and withers. This metaphor haunted pictorial representations of kinship for centuries until it finally assumed the fixed image of 'the family tree'," so writes Christiane Klapisch- Zuber in an essay about the origins of the family tree as we know it today. [1]
Example: My Family and I Essay in 500 words. Family plays an important role in our development. We are not always cognizant of the wide-reaching impact our parents, siblings, and extended family have on us as we grow—for good or ill. So, in this essay, my family and their impact on me is my chosen subject.
Explore the art of penning the perfect family essay. Dive into personal memories, embrace family quirks, and craft a narrative that resonates. 🖋 ... Writing a Family Tree Dive into your roots! A family tree can be more than names and dates; it can narrate stories of ancestors, their challenges, achievements, and legacies. For instance, "When ...
6. Seek Out Help. Look for writers' groups and classes in your community. From online groups to friends and family members, having a community you can rely on for feedback and encouragement is essential. Reaching out can also lead to new research finds, important for sourcing the details in your stories.
Answer: You can write about family members, relations, values and traditions of your family. Write down the places from where your ancestors belong or the origin of your family. Also, mention the family reunion or gatherings or the occasions when you all get together. Question 3.
Personal knowledge can form the first limbs of your family tree. Begin at home by gathering and organizing your papers, make a simple chart or list, beginning with you, your parents, grandparents, and great-grandparents. Search for the following: birth, baptismal, graduation, marriage, military, and occupational records
Who to Add and Who to Leave Out. Last Updated August 30, 2020. Make Instant Discoveries About Your Ancestors Here. The term family tree is defined as "a diagram showing the relationships between people in several generations of a family.". Add your parents, grandparents and great grandparents and you're well on your way to building your ...
A family or evolutionary tree represents a conventional structure that shows the relationships and documents common ancestry (Mader and Windelspecht 654). The purpose of any family tree is to demonstrate a lineage and enhance a better understanding of a crucial organizing principle of biological modifications.
To some learners, crafting Family Tree papers comes easy; others need the help of various types. The WowEssays.com catalog includes professionally crafted sample essays on Family Tree and related issues. Most definitely, among all those Family Tree essay examples, you will find a paper that get in line with what you see as a worthy paper.
The family was a Christian family. They praised God and celebrated Christmas with their family. When Christine was a teenager she moved out of the house. By this time she met my father, John Fourmy. She had three kids with him. Sarah, Torin, and me. Sarah was born in the late 1990's.
My Family Tree Essay Example. Culture. It plays a huge role in our lives. It impacts the way that we live our lives in many ways. The clothes we wear, what we believe in, what kinds of foods we eat, and what languages we speak. Culture can also be greatly affected by where you live. That being said, some people associate with other cultures ...
Family Tree. My grandparents from my mother's side of the family were both born in China and resided in a small town their entire life. My grandmother—Po Po, goes by the name of Ling Tan; and my grandfather—Gung Gung, is called Chau Yi Chen. Both of them lived in the same village and were tied together through arrange marriage which is a ...
Browning 1 Claire Browning Professor Flowers UCCP 102 19 April 2017 Family Tree Essay Browning Family Tree I started this project with literally no idea of where my family comes from. I asked my mom and my dad about their heritage and my mom replied, "I have absolutely no idea," and my dad said, "I don't know, somewhere in Germany, I ...
Essay on My Family (Essay 8 - 750 Words) My family is the best gift I have got. A family can be simply said to mean a social group of different people in our society that includes one or more parents and also their children. In a family, every member of the family commits to other members of the family in a mutual relationship.
Family Analysis When looking at my family tree for the first time, I realized how restricted my view of my bloodline was. At most, I know two generations of my family. But first let's start with my main, separated family. My mother is Margaret Teresa Brown, born May 11th, 1963. My father is Willie Todd Brown, born October 1st, 1962.
An Essay On Family Life. 1063 Words5 Pages. There is a metaphor of "Family, like branches in a tree, we all grow in different directions, yet our roots remain as one" which illustrate family is closely interrelated. The healthier on family functioning, the stronger roots and branches for family members' growth, and vice versa.
500+ Words Essay on Tree. Tree Essay- Trees are our best friends because they clean the air we breathe. Likewise, they also clean the water and soil and ultimately make the earth a better place. It is also a fact that people who live near trees are healthier, fit, and happier than people who do not. Moreover, it is our responsibility to look ...